
Did you know that nearly one in four men will experience significant pelvic or urinary discomfort at some point? If you’re feeling pain now, you’re not alone.
That burning sensation, urgent need to go, or deep ache can be confusing and scary. It’s hard to know exactly what’s wrong.
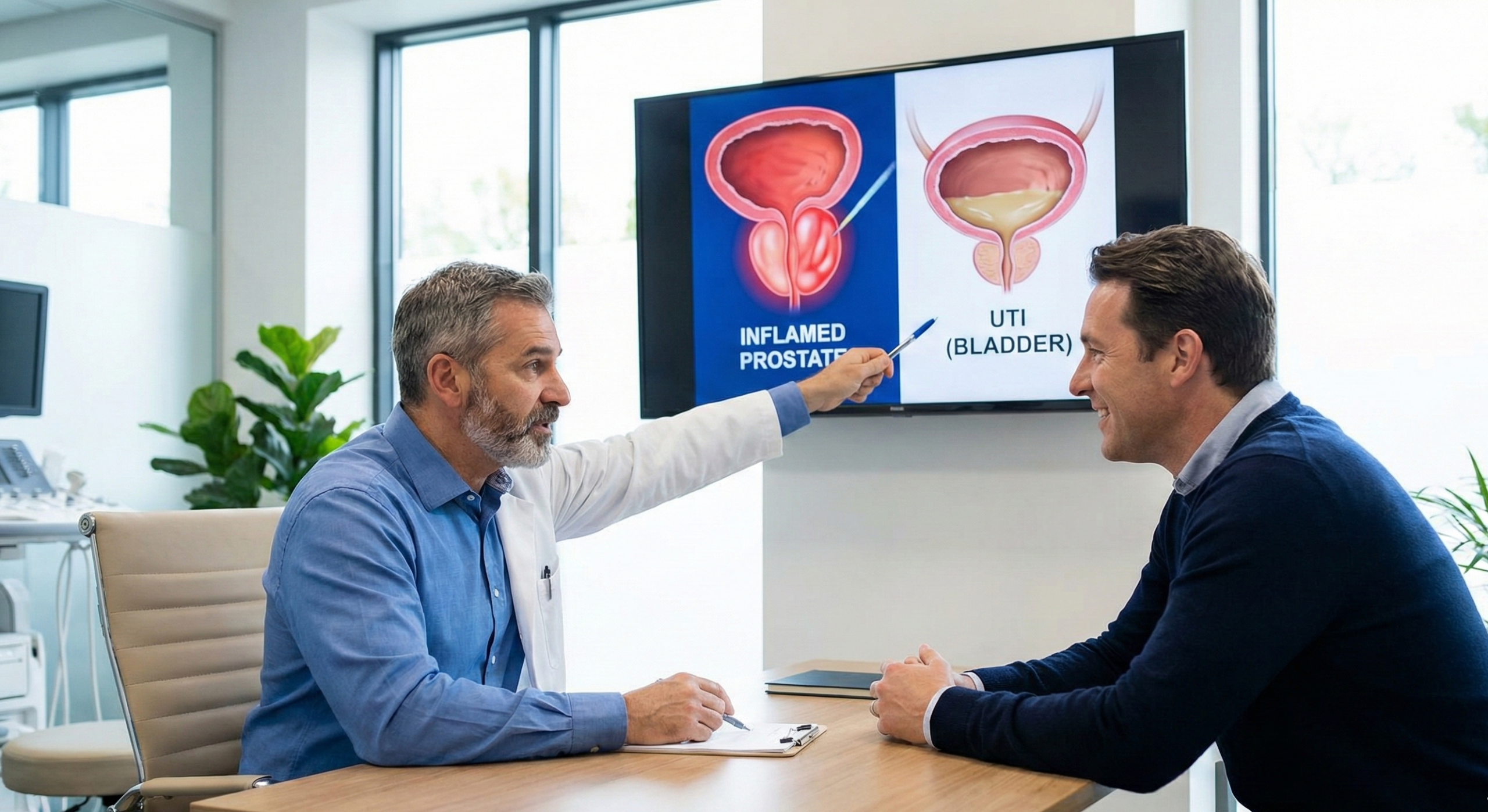
This guide is here to help. We’ll clearly explain the two most common culprits behind these symptoms: an inflamed prostate gland and a bacterial infection in the urinary system.
While their signs can seem similar, the causes and treatments are different. Getting the right information is your first step toward feeling better and taking back control of your prostate health.
Key Takeaways
- Pelvic and urinary pain in men is very common but often misunderstood.
- Two primary conditions cause these symptoms: Prostatitis (inflammation) and a urinary tract infection.
- These issues have overlapping signs, making self-diagnosis difficult.
- Understanding the root cause is critical for effective treatment and relief.
- This guide provides a detailed comparison to empower you with knowledge.
- Always consult a healthcare professional for an accurate diagnosis and personal treatment plan.
Understanding Pelvic and Urinary Pain in Men
When pain strikes below the belt, pinpointing its origin can feel like solving a complex puzzle. The male pelvic region contains interconnected organs and nerves. Discomfort in one area often signals trouble elsewhere.
At the center of many issues lies the prostate gland. This walnut-sized organ sits below the bladder and surrounds the urethra. When inflamed or irritated, it can trigger various symptoms throughout the region.
This pain doesn’t always stay in one place. You might feel it in your lower abdomen or groin. It can appear in the perineum, between the scrotum and rectum.
Some men experience discomfort at the tip of the penis or in the scrotum. The sensation often worsens during urination or ejaculation. This widespread pattern makes diagnosis challenging.
Referred pain adds another layer of confusion. A problem in the prostate can manifest as lower back ache. This happens because shared nerve pathways send signals to different areas.
Urinary changes usually accompany the physical discomfort. You might feel a sudden, strong need to urinate. Frequency increases, sometimes every hour or two.
Starting your stream may involve hesitation or difficulty. The flow can feel weak or stop and start. Many men report a feeling of incomplete emptying afterward.
These issues significantly impact daily life. Nighttime trips to the bathroom disrupt sleep. Sexual function may become affected or painful.
The constant pelvic pain creates background anxiety. It distracts from work and leisure activities. This psychological toll is real and deserves attention.
Medical professionals distinguish between acute and chronic presentations. Sudden, severe pain with fever requires immediate care. Persistent, nagging pelvic pain suggests a different cause.
Identical symptoms can stem from different sources. Painful urination might indicate an inflamed prostate. The same sensation could signal an infected bladder or urethra.
Understanding these nuances is crucial. It helps you communicate effectively with healthcare providers. Accurate description leads to proper diagnosis.
Research shows pelvic symptoms are surprisingly common. While this article focuses on men, similar issues affect many women. Knowing you’re not alone can provide some comfort.
The journey toward relief starts with comprehension. Recognizing patterns in your symptoms is the first step. Next, we’ll explore specific conditions that create these sensations.
What is Prostatitis? Inflammation of the Prostate Gland
The prostate gland plays a central role in many cases of male urinary and pelvic pain. This small organ sits just below your bladder. It surrounds the urethra, the tube that carries urine out of your body.
When this gland becomes inflamed, the condition is called Prostatitis. This inflammation can cause significant discomfort. It affects both urinary function and quality of life.
Think of your prostate as a walnut-sized gatekeeper. Its main job is producing fluid for semen. When swollen, it squeezes the urethra like a tight fist.
This pressure creates various symptoms. You might feel burning during urination. There could be pain in your groin or lower back.
Some men experience frequent urges to urinate. Others notice a weak stream. The sensation often feels deep within the pelvis.
The Four Types of Prostatitis
Medical experts classify this condition into four distinct categories. Each type has different causes and treatment approaches. Understanding which one you have is crucial.
Acute Bacterial Prostatitis is the most severe form. It comes on suddenly with intense symptoms. This type involves a confirmed bacterial infection.
You might experience high fever and chills. There can be severe pain between the scrotum and rectum. Urination becomes difficult and painful.
This condition requires immediate medical attention. Doctors typically prescribe strong antibiotics. Without treatment, complications can develop.
Chronic Bacterial Prostatitis features recurring infection. The symptoms are similar but less severe. They come and go over months or years.
This type often follows an acute episode. Bacteria hide deep within the prostate tissue. Standard antibiotic courses may not reach them effectively.
Chronic Pelvic Pain Syndrome (CPPS) is the most common form. It accounts for about 90% of all cases. Surprisingly, no standard bacterial infection is found.
The pain persists for at least three months. It centers in the pelvic region. Urinary and sexual dysfunction often accompany it.
Diagnosing CPPS involves ruling out other causes. Treatment focuses on managing symptoms. This approach differs from bacterial forms.
Asymptomatic Inflammatory Prostatitis shows no signs. Doctors discover it accidentally during other tests. Your prostate shows inflammation but causes no discomfort.
This type might be found during fertility evaluations. It can appear in prostate biopsies. Usually, no treatment is necessary.
| Type of Prostatitis | Primary Cause | Key Symptoms | Typical Duration | Treatment Approach |
|---|---|---|---|---|
| Acute Bacterial | Bacterial infection | Fever, chills, severe pain, urinary urgency | Sudden onset, short-term | Immediate antibiotics |
| Chronic Bacterial | Persistent bacterial infection | Recurrent pain, urinary symptoms, discomfort | Months to years | Long-term antibiotics |
| Chronic Pelvic Pain Syndrome (CPPS) | Non-bacterial (various theories) | Pelvic pain, urinary issues, sexual dysfunction | 3+ months | Multimodal symptom management |
| Asymptomatic Inflammatory | Unknown inflammation | None detected | Indefinite | Usually none required |
Common Causes and Risk Factors
Different types of this condition have different origins. Bacterial forms stem from identifiable sources. CPPS has more complex potential causes.
For bacterial Prostatitis, germs usually enter through the urinary tract. A bladder infection can spread to the prostate. Sexually transmitted organisms are another source.
Medical procedures sometimes introduce bacteria. Catheter use increases risk significantly. Any instrument in the urethra can carry germs.
Pelvic trauma from injury or surgery matters. It can damage local tissues. This creates pathways for bacteria to enter.
Chronic Pelvic Pain Syndrome puzzles researchers. Several theories explain its development. Pelvic floor muscle dysfunction is a leading idea.
These muscles may become too tight or spasm. They can irritate nearby nerves. This creates persistent pain signals.
Neurological factors also contribute. Nerves in the area might become oversensitive. They amplify normal sensations into pain.
Some evidence points to autoimmune responses. Your body might attack its own prostate tissue. Past infections could trigger this reaction.
Chemical irritation from urine is another theory. Certain substances might leak into prostate tissue. This creates ongoing inflammation.
Psychological stress plays a documented role. It can worsen muscle tension and pain perception. Stress management becomes part of treatment.
Several factors increase your overall risk. Previous urinary tract infections make recurrence likely. A history of Prostatitis raises chances significantly.
Pelvic region injuries create vulnerability. Medical procedures involving the urethra matter too. Age brings additional considerations.
Men over 50 often experience prostate changes. Enlarged prostate (BPH) is a separate condition. It doesn’t cause Prostatitis but can coexist.
It’s crucial to understand this distinction. Prostatitis involves inflammation or infection. BPH involves non-cancerous growth of the gland.
Many men worry about cancer connections. Research shows no direct link exists. Prostatitis does not cause prostate cancer.
It doesn’t increase your cancer risk either. The inflammation might temporarily elevate PSA levels. This can cause false alarms during screening.
Knowing these facts provides peace of mind. You can address your current symptoms without cancer fear. Proper diagnosis remains essential.

What is a UTI? A Urinary Tract Infection Explained
The male urinary tract has unique anatomical features that influence how infections develop and progress. A urinary tract infection occurs when bacteria invade any part of this system. In men, it most commonly affects the bladder (cystitis) and the urethra (urethritis).
Your urinary tract includes kidneys, ureters, bladder, and urethra. This pathway filters waste from your blood to create urine. It then stores and eliminates this fluid from your body.
Men have a longer urethra than women. This anatomical difference provides some protection. Bacteria must travel farther to reach the bladder.
This makes urinary tract infections less common in men. However, when they do occur, they are often more serious. The infection may indicate an underlying issue.
Statistics show these infections affect 40-60% of women at least once. About 26-44% experience recurrence within six months. Diagnosis can be complicated by unreliable testing methods.
The primary cause is usually bacteria entering through the urethra. Escherichia coli (E. coli) is the most common culprit. These germs normally live in the intestinal tract.
They can spread to the urinary opening. From there, they travel upward into the bladder. Once established, they multiply and cause an infection.
Several factors increase risk specifically for men. An enlarged prostate can obstruct urine flow. This creates stagnant fluid where bacteria can grow.
| Risk Factor | How It Increases Risk | Prevention Considerations |
|---|---|---|
| Enlarged Prostate (BPH) | Obstructs urine flow, causing retention | Manage prostate health, empty bladder fully |
| Kidney Stones | Create blockages and harbor bacteria | Stay hydrated, follow stone-prevention diet |
| Urinary Catheters | Provide direct pathway for bacteria | Maintain strict catheter hygiene |
| Recent Urinary Procedures | Can introduce bacteria or cause irritation | Follow post-procedure care instructions |
| Suppressed Immune System | Reduces ability to fight infections | Manage underlying conditions, boost immunity |
| Anatomical Abnormalities | May cause urine reflux or retention | Seek urological evaluation if recurrent |
Classic symptoms include a strong, persistent urge to urinate. You may feel burning during urination (dysuria). Many pass frequent, small amounts of urine.
The urine itself often appears cloudy. It may have a strong, unpleasant odor. Sometimes, it contains visible blood.
Pelvic pain or pressure can accompany these symptoms. Discomfort may center above the pubic bone. This happens as the inflamed bladder irritates surrounding tissues.
While typically straightforward, a urinary tract infection in men can signal deeper problems. It might indicate an underlying prostate issue. Anatomical abnormalities could also be present.
If untreated, the infection can ascend to the kidneys. This condition is called pyelonephritis. It represents a more serious medical situation.
Kidney infections cause additional symptoms. High fever and chills often develop. Flank pain (side pain below ribs) is common.
Nausea and vomiting may occur. The urine might contain pus. This requires prompt antibiotic treatment.
Recurrent utis in men warrant thorough evaluation. A urologist will check for contributing factors. These cases often involve more than simple bacteria.
Possible underlying causes include chronic prostate inflammation. Bladder outlet obstruction might be present. Complete assessment ensures proper management.
Remember that urinary tract infections and sexually transmitted infections share some symptoms. Both can cause pelvic discomfort. Accurate testing distinguishes between them.
If you experience these signs, consult a healthcare provider. They can perform appropriate tests. Early treatment prevents complications.
Prostatitis vs. UTI: A Side-by-Side Symptom Comparison

When urinary and pelvic symptoms appear, comparing their specific patterns is your most powerful tool for understanding. This detailed breakdown will help you see where the signs align and where they diverge.
Seeing the symptoms listed together clarifies the picture. It moves you from general worry toward specific knowledge.
Symptom Comparison Table
The table below organizes the common signs by category. It accounts for the different types of prostate inflammation.
| Symptom Category | Prostatitis (Varies by Type) | Urinary Tract Infection (UTI) |
|---|---|---|
| Primary Pain & Discomfort | Deep pelvic ache, pain in perineum (between scrotum & rectum), lower back pain, genital pain. Often a persistent “heavy” feeling. Pain during/after ejaculation is a hallmark. | Burning sensation centered in the urethra during urination (dysuria). Pressure or pain above the pubic bone (bladder area). |
| Urinary Symptoms | Frequent urination, urgency, weak stream, hesitancy, feeling of incomplete emptying. Difficulty starting or maintaining flow. Nocturia (nighttime urination). | Strong, persistent urgency to void. Frequent passing of small urine amounts. Cloudy, dark, or foul-smelling urine. May contain visible blood. |
| Systemic Symptoms | Acute bacterial type: High fever, chills, body aches, nausea. Other types: Typically no fever. | Lower UTI: Usually no fever. If infection reaches kidneys (pyelonephritis): High fever, chills, flank pain, nausea. |
| Onset & Duration | Acute: Sudden, severe. Chronic bacterial: Recurrent episodes. CPPS: Persistent pain lasting 3+ months. | Often develops over hours to days. Treated episodes typically resolve within a week. Recurrent utis may indicate an underlying cause. |
Key Overlaps and Critical Differences
Understanding both the similarities and the distinctions is crucial. Here’s what you need to know.
Where They Overlap:
- Both conditions can cause urinary frequency and a sudden, strong urge to go.
- Pelvic discomfort or a general sense of pressure is common to both.
- These shared symptoms are exactly why confusion happens.
Where They Diverge:
- Pain Location & Type: Prostate-related pain is often more diffuse—spreading to the genitals, lower back, or perineum. UTI discomfort is tightly focused on the act of urination and the bladder area.
- Sexual Function: Pain during or after ejaculation is a strong indicator of an inflamed prostate, not a typical urinary tract infection.
- Urine Appearance: Cloudy or foul-smelling urine is a classic sign of a bacterial infection like a UTI. This is less consistent in non-bacterial prostate conditions.
- Systemic Signs: The presence of a high fever and chills is a major red flag. It strongly points to acute bacterial prostate inflammation or a kidney infection, requiring immediate medical care.
- Timeline: Chronic Pelvic Pain Syndrome (CPPS) involves persistent pain lasting months. Most infections are acute, with symptoms that come on more sharply.
Let this guide your next steps. Severe pain with fever demands an emergency visit. For persistent or confusing symptoms, schedule a doctor’s appointment for a precise diagnosis.
How Doctors Diagnose the Source of Your Pain
A precise diagnosis is the critical bridge between confusing symptoms and effective treatment. Healthcare providers follow a logical sequence to identify the root cause of your discomfort.
This process eliminates guesswork. It provides clarity and direction for your recovery journey.
The Initial Consultation and Physical Exam
Your first appointment focuses on gathering detailed information. The doctor will ask specific questions about your experience.
They need to know when your symptoms began. Be ready to describe their pattern and intensity.
Common questions cover urinary frequency and urgency. You’ll discuss any pain during urination or ejaculation.
The physician will inquire about fever or chills. They’ll ask if you notice changes in your urine appearance.
This conversation helps narrow down potential conditions. Honest answers lead to better diagnosis accuracy.
Next comes the physical examination. The digital rectal exam (DRE) assesses your prostate gland directly.
During this quick procedure, the doctor inserts a gloved finger into the rectum. They check for swelling, tenderness, or unusual texture.
The exam provides immediate feedback about prostate size and consistency. Many men feel anxious about this step.
Remember it’s a routine clinical assessment. It lasts less than a minute and offers valuable information.
Essential Diagnostic Tests
Laboratory tests provide objective data about your health. They confirm or rule out specific conditions.
Urinalysis examines a urine sample under a microscope. It looks for white blood cells indicating inflammation.
This test also detects red blood cells or unusual particles. Results come back within hours.
A urine culture takes the analysis further. It identifies specific bacteria causing an infection.
The culture determines which antibiotics will work best. This guides targeted treatment decisions.
Blood tests offer additional insights. A complete blood count checks for signs of systemic infection.
The PSA (prostate-specific antigen) test measures a protein from the prostate gland. Elevated levels can signal inflammation.
PSA screening also helps rule out prostate cancer. Remember that inflammation alone raises PSA temporarily.
An elevated result doesn’t mean you have cancer. It prompts further investigation.
For complex cases, urologists order advanced tests. A transrectal ultrasound creates images of the prostate.
It visualizes the gland’s structure and size. This helps identify abscesses or unusual growth.
Cystoscopy involves inserting a thin camera into the urethra. The doctor examines the urinary tract lining directly.
This procedure checks for strictures or other abnormalities. It’s typically done with local anesthesia.
Suspected chronic pelvic pain requires specialized evaluation. The “four-glass” test collects different fluid samples.
It compares urine before and after prostate massage. This localizes the source of inflammation or infection.
A simpler version uses two samples. Both methods help distinguish between types of chronic issues.
Diagnosis often involves ruling out other possibilities. This “diagnosis by exclusion” confirms chronic pelvic pain syndrome.
It ensures no bacterial cause or structural problem exists. Only then can appropriate management begin.
Prepare for your medical visit by tracking symptoms. Note their timing, triggers, and severity patterns.
Be open about sexual function concerns. This information is crucial for accurate assessment.
Bring a list of medications and supplements. Share your complete health history honestly.
These steps empower your healthcare team. They lead to a precise understanding of your situation.
Conventional Treatment Paths for Prostatitis

Receiving a clear diagnosis marks the beginning of your journey toward effective symptom management. Modern medicine offers structured approaches tailored to the specific type of prostate inflammation you have.
The right treatment plan depends entirely on whether harmful bacteria are present. Your doctor will determine this through urine tests and clinical evaluation.
Two main pathways exist for addressing this condition. Bacterial forms require antimicrobial strategies. Non-bacterial chronic issues need multimodal management.
Understanding these options empowers you to participate actively in your care. You can ask informed questions during medical consultations.
Treating Bacterial Prostatitis: The Role of Antibiotics
When tests confirm a bacterial infection, antibiotics become the cornerstone of treatment. These medications eliminate the germs causing your symptoms.
Doctors prescribe different regimens for acute and chronic cases. The duration reflects how deeply bacteria can hide in prostate tissue.
Acute bacterial prostatitis demands immediate attention. This is considered a urological emergency.
You may experience high fever and severe pain. Hospitalization is often necessary for close monitoring.
Intravenous (IV) antibiotics deliver strong medication directly into your bloodstream. This ensures rapid control of the spreading infection.
After a few days, you typically transition to oral medications. The complete course usually lasts 14 to 30 days.
Chronic bacterial prostatitis involves persistent or recurring issues. Bacteria embed themselves in the prostate‘s complex structure.
Poor blood flow to the gland makes treatment challenging. Standard short courses often fail to reach all hidden germs.
For this reason, doctors prescribe much longer antibiotic regimens. You might take medications for 4 to 12 weeks continuously.
Completing the entire prescribed course is absolutely critical. Stopping early allows surviving bacteria to multiply again.
Common antibiotic classes used include:
- Fluoroquinolones (like ciprofloxacin or levofloxacin)
- Trimethoprim-sulfamethoxazole (Bactrim, Septra)
- Tetracyclines (like doxycycline)
Your doctor selects the specific drug based on test results. Culture reports show which bacteria are present and what kills them best.
Some men experience side effects from prolonged antibiotic use. Discuss any concerns with your healthcare provider promptly.
Managing Chronic Pelvic Pain Syndrome (CPPS)
Most cases of persistent prostate inflammation show no bacterial cause. This condition, called Chronic Pelvic Pain Syndrome, requires a different strategy.
The gold standard approach is the UPOINT system. This multimodal framework addresses six key domains contributing to symptoms.
Research shows approximately 80% of people improve significantly with this personalized method. It treats you as a whole person, not just a diagnosis.
| UPOINT Domain | Primary Focus | Common Treatment Options | Rationale |
|---|---|---|---|
| Urinary | Bladder and urinary symptoms | Alpha-blockers (tamsulosin), anticholinergics | Relaxes muscles, improves flow, reduces urgency |
| Psychosocial | Stress, anxiety, depression | Cognitive behavioral therapy, stress management, counseling | Reduces tension that worsens pelvic muscle spasms |
| Organ-specific | Prostate inflammation | Supplements (quercetin, bee pollen, cernilton) | May reduce inflammatory markers in the gland |
| Infection | Possible hidden infection | Empirical antibiotics (sometimes used) | Controversial practice when no bacteria are found |
| Neurological | Nerve-mediated pain | Low-dose antidepressants (amitriptyline), anti-seizure drugs (gabapentin) | Calms overactive nerves, treats neurogenic pain |
| Tenderness | Muscle spasms and tension | Pelvic floor physical therapy, myofascial release | Releases tight muscles causing referred pain |
Pelvic floor dysfunction is a central component for many men. These muscles can become chronically tight or spastic.
A specialized physical therapist teaches you relaxation techniques. They use internal and external massage to release trigger points.
This therapy often provides dramatic relief. It addresses the muscular component of your discomfort directly.
Neurological treatments target nerve damage or hypersensitivity. Medications like low-dose amitriptyline work on pain pathways.
They’re prescribed at doses much lower than for depression. The goal is to calm amplified pain signals from the pelvic region.
The “Infection” domain remains controversial in UPOINT. Some doctors prescribe antibiotics even without proof of bacteria.
This empirical approach assumes possible hidden infection. Not all experts agree with this practice.
If your doctor suggests this, ask about their reasoning. Understand the potential benefits versus risks of long-term medication.
Procedural options exist for certain situations. Prostate massage aims to drain congested ducts within the gland.
A urologist performs this during a rectal examination. Some studies suggest regular ejaculation may offer similar benefits.
Always discuss procedural interventions with your specialist. They can explain whether you’re a good candidate.
Over-the-counter pain relievers help manage flare-ups. Prescription medications target more severe discomfort.
Mental health support addresses the psychological toll. Chronic pelvic pain affects mood, sleep, and relationships.
A comprehensive approach yields the best results. Combining multiple strategies attacks the problem from different angles.
Work closely with your healthcare team to customize your plan. What helps one person might differ for another.
Conventional Treatment Paths for UTIs
Medical professionals approach urinary tract infections in men with specific protocols designed for effective resolution. Standard care focuses on eliminating the harmful microorganisms causing your discomfort.
For an uncomplicated case, your doctor typically prescribes a short course of oral medication. This usually lasts three to seven days.
Common antibiotics include trimethoprim-sulfamethoxazole, nitrofurantoin, or fluoroquinolones. The choice depends on local resistance patterns and your medical history.
Taking your medication exactly as directed is absolutely critical. Complete the entire prescribed course even if symptoms disappear quickly.
Stopping early allows surviving bacteria to multiply again. This leads to recurrence and promotes antibiotic resistance.
“Finishing your full antibiotic course is non-negotiable. Partial treatment creates the perfect environment for stronger, drug-resistant bacteria to emerge.”
Urine culture results play a vital role in guiding treatment. If the first medication doesn’t work, the culture identifies a more effective alternative.
This laboratory test shows which specific germs are present. It also reveals which drugs will eliminate them most efficiently.
Managing Recurrent Infections
Frequent infections require different strategies. Your healthcare provider may recommend longer antibiotic courses lasting two to four weeks.
Low-dose preventive antibiotics represent another option. You might take these daily or after sexual intercourse.
Investigating underlying causes becomes essential with recurrent issues. Prostate inflammation or anatomical abnormalities could be contributing factors.
| Treatment Scenario | Standard Approach | Duration | Key Considerations |
|---|---|---|---|
| First-time, Uncomplicated | Short-course oral antibiotics | 3-7 days | Based on likely pathogens; complete full course |
| Recurrent Infection | Longer antibiotic course OR preventive therapy | 2-4 weeks OR ongoing low-dose | Must investigate underlying causes (e.g., prostate issues) |
| Culture-Guided Therapy | Antibiotics selected based on urine culture results | Varies by case | Used when initial treatment fails or for complicated cases |
| Symptom Management | Phenazopyridine (Pyridium) alongside antibiotics | Short-term only (2-3 days) | Provides temporary bladder pain relief; doesn’t treat infection |
Symptom Relief and Home Remedies
Medications like phenazopyridine can numb bladder pain temporarily. These provide comfort while antibiotics work to clear the infection.
Remember these relief options don’t treat the underlying problem. Use them only as directed for short periods.
Cranberry juice remains a popular home remedy among many people. Scientific evidence for treating active utis in men is weak.
While it might offer some preventive benefits, it should never replace prescribed medication. Always consult your doctor before trying alternative approaches.
Special Considerations for Men
Medical guidelines consider any urinary tract infection in a male patient as “complicated.” This classification warrants thorough follow-up care.
Your provider needs to ensure complete resolution. They should also investigate potential root causes.
Follow-up testing confirms the infection is fully cleared. A “test of cure” urine culture provides this verification.
This extra step is particularly important for recurrent utis. It helps prevent future episodes and identifies any persistent issues.
Successful treatment combines appropriate medication with proper follow-up. Addressing both aspects ensures lasting relief and reduces recurrence risk.
At-Home Strategies for Symptom Relief and Management

Your home environment offers powerful tools for managing symptoms alongside professional medical care. These approaches provide supportive relief while your body heals or during ongoing treatment.
Think of these strategies as your personal toolkit. They help reduce daily discomfort and improve your quality of life. Consistency is key for seeing the best results.
Remember these methods complement, but don’t replace, doctor-prescribed treatments. They work well for chronic pelvic pain syndromes and general symptom relief.
Hydration and Dietary Adjustments
What you drink and eat directly affects urinary and pelvic comfort. Making smart choices can significantly reduce irritation.
Water is your best friend for urinary health. Aim for six to eight glasses daily to dilute your urine.
This reduces burning during urination and helps flush out irritants. Proper hydration promotes regular bladder emptying.
Some beverages and foods can worsen symptoms. Consider limiting or avoiding these common triggers.
| Category | Items to Limit or Avoid | Why They Can Worsen Symptoms | Better Alternatives |
|---|---|---|---|
| Beverages | Coffee, black tea, soda, alcohol | Act as diuretics or bladder irritants; can increase urgency and frequency | Water, herbal tea, diluted fruit juice |
| Foods | Spicy dishes, citrus fruits, tomatoes, chocolate | May irritate the bladder lining or prostate tissue; can increase inflammation | Bananas, potatoes, whole grains, lean proteins |
| Additives | Artificial sweeteners, MSG, excessive salt | Can trigger pelvic muscle spasms or fluid retention | Natural herbs, small amounts of honey or maple syrup |
| Potential Helpers | Pumpkin seeds, green tea, alkaline water | May soothe the bladder; some contain anti-inflammatory compounds | Incorporate in moderation as part of balanced diet |
Start by eliminating one group at a time. This helps identify your personal triggers without overwhelming changes.
Keep a simple food diary for two weeks. Note what you consume and any changes in your symptoms.
Many people find relief within days of adjusting their diet. The effects are often noticeable and encouraging.
Lifestyle and Behavioral Modifications
Daily habits and physical adjustments offer another layer of relief. These techniques address muscular tension and nervous system responses.
Warmth is remarkably effective for pelvic pain. A sitz bath or heating pad relaxes tight muscles in the lower back and perineum.
Soak in warm water for 15-20 minutes daily. This improves blood flow and eases deep muscular discomfort.
Stress directly impacts pelvic symptoms through the mind-body connection. Tension often settles in these muscles.
Practice relaxation techniques like deep breathing or meditation. Gentle yoga can release stored physical stress.
Your sitting position matters throughout the day. Consider a donut cushion if you sit for long periods.
This simple tool takes pressure off sensitive areas. It prevents worsening of existing pain during work or travel.
Choose loose, comfortable clothing over tight pants or underwear. Restricted blood circulation can aggravate symptoms.
Modify your exercise routine wisely. Avoid activities that put direct pressure on the pelvic region.
Cycling is a common trigger for many cases. Switch to walking, swimming, or light jogging instead.
These activities maintain fitness without aggravating your conditions. Listen to your body and adjust intensity as needed.
| Modification Area | Specific Strategy | How It Helps | Implementation Tips |
|---|---|---|---|
| Bladder Habits | Bladder training, double-voiding | Reduces urgency frequency; improves emptying to prevent retention | Delay bathroom visits gradually by 5-10 minutes; try urinating twice |
| Posture & Sitting | Donut cushion, regular standing breaks | Relieves perineal pressure; improves pelvic blood circulation | Use cushion for drives >30 minutes; stand up every hour |
| Stress Management | Meditation, deep breathing, gentle yoga | Reduces muscle tension; calms nervous system amplification of pain | Start with 5 minutes daily; use apps for guided sessions |
| Clothing Choices | Loose-fitting pants, breathable fabrics | Prevents constriction; reduces heat and moisture buildup | Avoid tight jeans; choose cotton underwear over synthetic |
| Exercise Modifications | Walking, swimming, avoid cycling | Maintains fitness without pelvic pressure; improves overall circulation | Start with 20-minute walks; consider water aerobics classes |
Bladder training helps with urgency and frequency symptoms. Gradually extend time between bathroom visits by a few minutes.
Double-voiding addresses incomplete emptying. Urinate, wait a moment, then try again to ensure your bladder is fully empty.
These behavioral changes require patience and practice. Start with one or two modifications that seem most relevant to your situation.
Track your progress in a simple journal. Note which strategies bring the most relief for your specific symptoms.
Over-the-counter pain relievers like ibuprofen can help during flare-ups. Always follow dosage instructions and consult your doctor about regular use.
Remember that these approaches work best alongside medical therapy. They address the lifestyle components of your health journey.
Most men find combining several strategies yields the best results. Customize your approach based on what works for your body.
Consistent application transforms these practices into lasting habits. They become part of your daily routine for ongoing comfort and wellness.
Natural Management and Long-Term Prostate Support
For ongoing prostate support, a holistic approach that includes evidence-based supplements can be valuable. These natural strategies focus on maintaining wellness after acute issues resolve.
They work alongside medical guidance for comprehensive care. Think of them as part of your long-term health maintenance plan.
The Role of Evidence-Based Supplements
Certain natural compounds show promise for supporting prostate comfort. Research highlights specific ingredients that may help reduce inflammation.
Quercetin is a bioflavonoid with strong anti-inflammatory properties. Studies suggest it can benefit some men with chronic pelvic discomfort.
Bee pollen extracts, like cernilton, also demonstrate potential. These supplements may help relieve swelling in the prostate gland.
ProstaLite represents a comprehensive formula combining researched ingredients. This highly-rated supplement includes Saw Palmetto and Uvaria Rufa.
Saw Palmetto (serenoa repens) is widely recognized for prostate support. It may help shrink inflamed tissue and improve urinary flow.
Uvaria Rufa is another botanical with traditional use for urinary comfort. Together, these ingredients target multiple aspects of prostate health.
These supplements are designed for long-term maintenance, not acute infection treatment. They support your body’s natural processes over time.
Other Supportive Natural Compounds
Several additional natural options may contribute to prostate wellness. Each works through different mechanisms in the body.
Pygeum Africanum comes from African plum tree bark. It contains compounds that may support urinary function and comfort.
Stinging Nettle root has been used traditionally for urinary issues. Some research suggests it helps with symptoms of an enlarged prostate.
Zinc is an essential mineral for prostate health. The gland contains high concentrations of this important nutrient.
Lycopene, found in tomatoes, is a powerful antioxidant. It helps protect cells from oxidative damage throughout the body.
These compounds address various aspects of prostate function. They support the gland’s structure and reduce inflammatory responses.
Important considerations for supplement use:
- Supplements are not first-line treatments for active infections
- They work best as part of a comprehensive wellness strategy
- Quality and dosage vary significantly between products
- Natural doesn’t always mean safe for everyone
Critical Disclaimer: Always consult your healthcare provider before starting any supplement. Discuss potential interactions with medications you’re taking.
Your doctor can ensure supplements are appropriate for your specific condition. They’ll consider your overall health and any underlying causes.
This professional guidance helps avoid unwanted side effects. It ensures your approach supports rather than conflicts with medical treatment.
Regular check-ups and tests remain essential for monitoring prostate health. These appointments catch any changes early.
Natural management complements but doesn’t replace professional medical care. Together, they form a complete approach to long-term wellness.
Conclusion: Taking the Next Step Toward Relief
Understanding your symptoms is the first powerful step toward reclaiming your comfort and health. While pelvic and urinary issues can seem similar, they stem from different sources.
An accurate professional diagnosis is essential. Use what you’ve learned here to have an informed talk with your doctor.
Both conditions are manageable with the right approach. This includes targeted medical treatment and supportive lifestyle changes.
Don’t ignore persistent pain or discomfort. Seeking help shows you value your wellbeing. Take charge of your prostate and urinary health today.
👉 Check ProstaLite Availability & Read Reviews
FAQ
Can I treat what I think is a UTI with leftover antibiotics?
No, you should never use leftover antibiotics. This is dangerous and often ineffective. What feels like a simple bladder infection could be Prostatitis, which requires a different, longer antibiotic course. Taking the wrong medication can worsen your condition and contribute to antibiotic resistance. Always see a doctor for a proper diagnosis.
Is pain during or after ejaculation a sign of a urinary tract infection?
Typically, no. Pain with ejaculation is a hallmark symptom of Prostatitis, especially chronic pelvic pain syndrome (CPPS). While a severe UTI might cause general discomfort, ejaculatory pain points directly to inflammation in the prostate gland. Mentioning this specific symptom to your doctor is a key clue for an accurate diagnosis.
How long does it take to get better from prostatitis compared to a UTI?
A> Recovery times differ greatly. An uncomplicated bladder infection often clears within a few days of starting the correct antibiotics. Bacterial Prostatitis, however, usually requires a minimum of 4 to 6 weeks of medication. For chronic pelvic pain syndrome (CPPS), management is a longer-term process focused on controlling symptoms and improving quality of life, not just a quick cure.
Can an untreated UTI turn into prostatitis?
Yes, this is possible. Bacteria from an untreated urinary tract infection can travel up the urethra and infect the prostate gland, causing acute bacterial Prostatitis. This is a serious condition that often comes with high fever and chills. It highlights why promptly treating any suspected bladder infection is crucial for your health.
Are there specific tests to rule out prostate cancer when I have these symptoms?
A> While prostate cancer can sometimes cause urinary symptoms, the pain and urgency from Prostatitis or a UTI are usually different. Your doctor will likely perform a digital rectal exam to feel the gland. If they find irregularities or based on your risk factors, they may order a PSA blood test. It’s important to discuss all your symptoms to guide appropriate testing.
What lifestyle changes help manage chronic pelvic pain from prostatitis?
A> Several adjustments can provide relief. Avoiding bladder irritants like caffeine, alcohol, and spicy foods is a good start. Regular warm baths can ease muscle tension. Stress management techniques and specialized physical therapy that focuses on relaxing the pelvic floor muscles are often core parts of a successful long-term management plan for this condition.


“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”

