Surprising fact: Some studies suggest that up to one in three men may experience urinary leakage by midlife, yet many believe nothing can help.
This guide explains a targeted way to train the pelvic floor muscles to support the bladder and reduce stress leakage during coughing or lifting.
The approach is skill-based: finding the right muscles matters. Progress is gradual, like strengthening any other muscle. Results vary and may take weeks of consistent practice.
The guide covers what pelvic floor muscles do, likely benefits and realistic outcomes, how to locate the correct muscles, a step-by-step technique, building a routine, and safety flags to watch for.
Aim for safer, more effective practice by avoiding common mistakes such as squeezing the buttocks or holding the breath, which reduce benefit.
Medical note: persistent or worsening urinary symptoms, pain, or new bowel or sexual concerns should be discussed with a clinician to rule out other causes.
Key Takeaways
- Pelvic floor training targets muscles that support bladder control.
- Learning the right technique is essential; progress is usually gradual.
- Common users include those with urgency, leakage, or post-prostate changes.
- Practice safely: avoid breath-holding, straining, and buttock squeezing.
- See a clinician if symptoms persist, worsen, or are accompanied by pain.
Understanding the pelvic floor muscles and why they matter
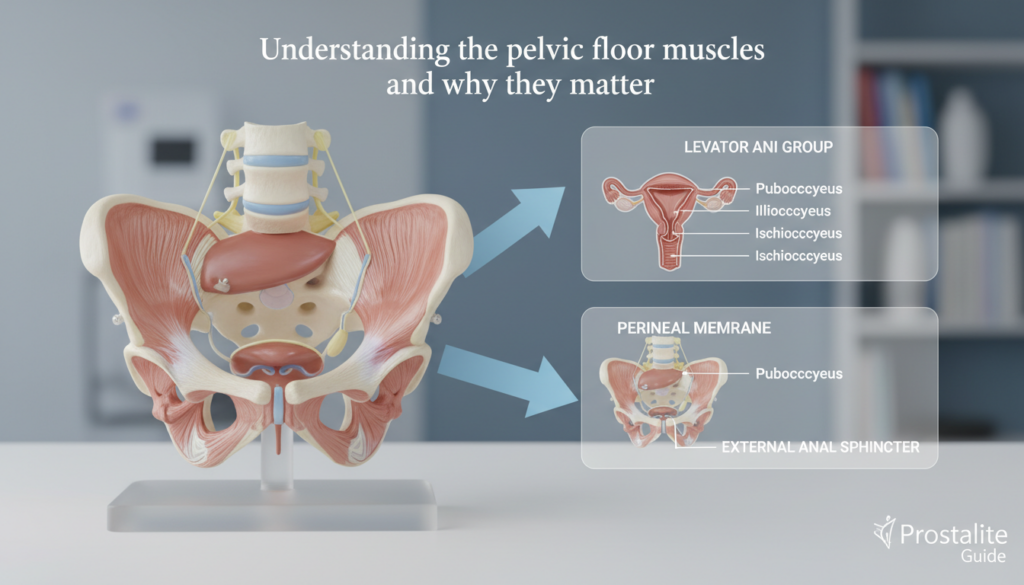
The pelvic floor acts like a supportive hammock at the base of the pelvis. It is made of layered pelvic floor muscles that hold pelvic organs and help control both urine and stool.
What the pelvic base supports
The pelvic floor supports the bladder, bowel, and urethra. The bladder stores urine. The urethra is the tube that carries urine out. Sphincter and floor muscles tighten to stop flow and relax to allow voiding.
Symptoms versus possible causes
People notice symptoms like leakage or sudden urgency to pass urine. These are signs, not a single diagnosis.
Pelvic floor weakness can contribute to leakage, but other causes include bladder irritation, medications, infection, or prostate-related change.
Common risk factors that weaken the floor
- Aging and periods of low activity that reduce muscle tone.
- Pelvic surgery or prostate treatment such as surgery or radiation.
- Chronic coughing or straining with constipation that stresses the floor muscles.
Why this matters: clinicians may recommend pelvic floor strengthening as a conservative option. Accurate evaluation is important when symptoms are new or severe.
Benefits and realistic expectations for pelvic floor exercise

Targeted pelvic muscle work often leads to steady improvement in bladder control over weeks to months. Clinical guidance and trials note that training can lessen urine leakage for many men, especially after prostate treatment, but outcomes vary by individual.
How training may reduce incontinence episodes
Training aims to strengthen pelvic floor muscles and improve coordination so muscles hold urine in place during activities such as coughing or lifting.
“Studies show pelvic floor training can reduce the frequency and volume of leakage and improve quality of life for many people.”
What “reduced incontinence” can look like:
- Fewer accidental leaks.
- Smaller amounts when leaks occur.
- More confidence during movement and less avoidance of activities.
Stronger pelvic muscles may help erectile function or orgasmic sensation for some, but results depend on nerve health, overall health, and prior prostate care.
| Benefit | Timeline | Notes |
|---|---|---|
| Reduced leakage | Weeks to months | Often gradual; track frequency and pad use |
| Improved control | 6+ weeks | May need combined therapies (bladder training, meds) |
| Sexual support | Variable | Depends on nerve and prostate treatment history |
When to see a clinician: seek evaluation for persistent or worsening symptoms, pain, blood in urine, fever, or sudden severe urgency rather than relying on self-care alone.
How to find the right muscles before starting

Identifying the correct pelvic region is the first practical step toward useful muscle training. He should learn simple cues to sense the small internal lift that matters.
Simple cues to try
Briefly try to stop the urine stream or imagine holding back passing gas. These actions give a useful signal to the pelvic floor muscle without becoming the main method.
How the correct contraction feels
- Sensation: a small inward lift and gentle squeeze, not a hard clench of the buttocks or thighs.
- Avoid: pushing downward or tensing abdominal or leg muscles — these are the wrong muscles and reduce benefit.
- Optional cue: gently lifting the scrotum upward may help some men feel the floor muscle engage.
Testing safely and next steps
Do not repeatedly stop-start the urine stream. Frequent interruption of the urine stream can irritate the bladder and change normal emptying.
If he cannot reliably find the right muscles, a clinician or pelvic floor physical therapist can help with assessment and hands-on cues like a rectal finger check if comfortable.
Kegel Exercises for Men: Step-by-Step Technique

Begin with simple positions that let him feel a clear, gentle internal lift before moving to upright tasks.
Best starting positions and progression
Start lying on the back or side with knees slightly bent, or sit with feet flat and lumbar support. These positions reduce strain and make sensing the lift easier.
Progress to standing once control is reliable, since standing matches many daily triggers.
Proper contraction checklist
- Lift and squeeze internally; feel a small upward pull.
- Keep the stomach soft and breathe normally.
- Do not tighten buttocks or squeeze thighs.
- Avoid pushing downward; reset if other muscles engage.
Timing and session structure
Hold the contraction for five seconds, counting out loud to avoid breath-holding, then fully relax for five seconds. Aim for ten repetitions per session and repeat sessions several times a day.
Gradually increase holds toward ten seconds on and ten seconds off only if comfortable and symptom-free. Stop early if the pelvic floor muscles fatigue or if there is pain, and seek clinical advice for persistent discomfort.
How often to do Kegels and when to use them in daily life
Small, consistent practice at predictable times helps the pelvic floor adapt to daily demands. Aim for short sessions rather than one long effort. Quality and regularity matter more than volume.
Typical daily routine
Practical plan: start with ten repetitions per session and repeat that set at least three times a day — morning, afternoon, and evening. Count a five-second hold with a five-second rest, or shorter holds if fatigue appears.
Using a contraction before common triggers
Teach the body to brace before movement. Do a quick, gentle contraction just before coughing, laughing, lifting, standing up, or starting to walk. This “before a trigger” cue can reduce stress leakage during routine actions.
What to expect over time
Early change is often subtle. Meaningful strengthening typically takes six weeks or longer. He should track urine leaks and triggers to spot patterns and share them with a clinician if progress stalls.
“Consistency over weeks usually gives the best chance of improved bladder control.”
Make the habit discreet: contract while fastening a seatbelt, before rising from a chair, or when picking up groceries. If urgency or increased leakage continues or worsens, seek medical assessment — pelvic weakness is only one possible cause.
Safety tips and signs something isn’t right
Knowing red flags and simple posture checks keeps practice safe and effective.
Do not use a catheter during practice
Do not do kegel exercises while a Foley catheter is in place. Clinical guidance warns this can cause bleeding or bladder spasms and harm urinary health.
Red flags to stop and reassess
If contractions cause pain, pelvic or abdominal discomfort, new or worse leakage, or sudden urgency, stop and rest.
Headache during practice often means breath-holding. Back or stomach pain may mean the body is using the wrong muscles.
Breathing and posture checks
- Keep ribs and shoulders relaxed; breathe out gently during each squeeze.
- Avoid pushing down as if starting a bowel movement; do a small internal lift instead.
- Stop when the pelvic floor feels tired—soreness is not the goal.
When to contact a clinician or seek therapy
Talk to a healthcare provider if he cannot find the pelvic floor muscles, has persistent incontinence, major urine changes, or concerns after prostate care.
Referral to pelvic floor physical therapy is appropriate when self-guided practice is unclear or not helping; therapists can use biofeedback, relaxation, and manual methods tailored to individual needs.
Considering additional support
Some men choose to explore dietary supplements as part of a broader routine to support prostate and urinary comfort. If you are considering this option, you can learn more about ProstaLite here.
It’s important to note that supplements are not a substitute for medical care or proper pelvic floor training. Results vary, and anyone with ongoing or worsening symptoms should speak with a healthcare professional before starting any new product.
Conclusion
A short, consistent routine can help him gain better control over urine over weeks without special equipment.
Pelvic floor training is a practical, low-cost skill that may help strengthen pelvic support when the correct muscles are used and the core stays relaxed.
The key steps are simple: find the pelvic floor muscles, contract with a gentle lift, breathe normally, and fully relax between reps. Progress slowly and avoid pain.
Use a quick lift just before coughing, lifting, or standing to reduce leaks, while keeping dedicated practice sessions to build strength and coordination.
If symptoms persist, worsen, or affect quality of life, he should consult a healthcare provider and consider pelvic floor physical therapy for tailored guidance and reassurance.
Trusted Resources for Further Reading
For more in-depth medical insights, we recommend consulting established health authorities. The Mayo Clinic provides a comprehensive overview of proper technique and benefits. Additionally, the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) offers extensive research on bladder control issues, while the Urology Care Foundation is an excellent resource for understanding broader urological health and treatment options.
FAQ
What do the pelvic floor muscles support in men?
How can someone tell if leakage and urgency are caused by weak pelvic floor muscles?
What common factors increase the risk of pelvic floor weakness?
How can pelvic floor training help bladder control and reduce incontinence?
Are there sexual health benefits, and will everyone see the same results?
What simple cues help locate the correct muscles before starting?
What do the “right muscles” feel like and how can someone avoid using the wrong ones?
Why should someone avoid testing by stopping urine flow often?
What are the best starting positions to practice pelvic contractions?
How should a proper contraction feel and what breathing pattern is advised?
What are the basic timing guidelines for holds and rests?
How many repetitions and sets make up a typical session, and when should someone stop?
How often should pelvic training be done and when is it most useful during daily life?
How long before someone notices improvement?
Why must these contractions not be done with a Foley catheter in place?
What warning signs indicate something isn’t right during practice?
How can someone prevent straining and pushing down while training?
When should a healthcare provider or pelvic floor physical therapist be consulted?

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”


