⚠️ Important Medical Note: This guide is for educational purposes. While we discuss natural support options, always consult a physician for persistent or severe symptoms.
Nearly half of older men report noticeable urinary changes by their seventies, a figure that shows how common this condition can be.
Everyday talk often calls this an enlarged prostate, and benign prostatic hyperplasia (BPH) is a frequent reason it develops over time.
This brief guide explains what growth of the gland means for urine flow and quality of life. It outlines the main biologic reasons, common risk factors, and typical symptoms seen in clinical care in the United States.
People vary: some have moderate enlargement with few complaints, while others feel marked symptoms even with small growth. Because of that variation, a clinician can help decide whether watchful waiting, testing, or treatment fits a person’s age and health.
Safety note: sudden inability to urinate, blood in the urine, or fever with painful urination are urgent signs. Seek immediate care if these occur.
Key Takeaways
- BPH is a common, benign reason the gland grows and can affect urination.
- Growth sits below the bladder and can narrow the urethra, changing flow.
- Symptoms like nighttime trips, urgency, or weak stream vary by person.
- Clinicians separate underlying mechanisms, risk factors, and symptoms to guide care.
- Seek urgent care for inability to urinate, visible blood, or fever with pain.
- This article is educational, not a diagnosis; consult a healthcare professional for persistent issues.
Understanding an enlarged prostate and benign prostatic hyperplasia
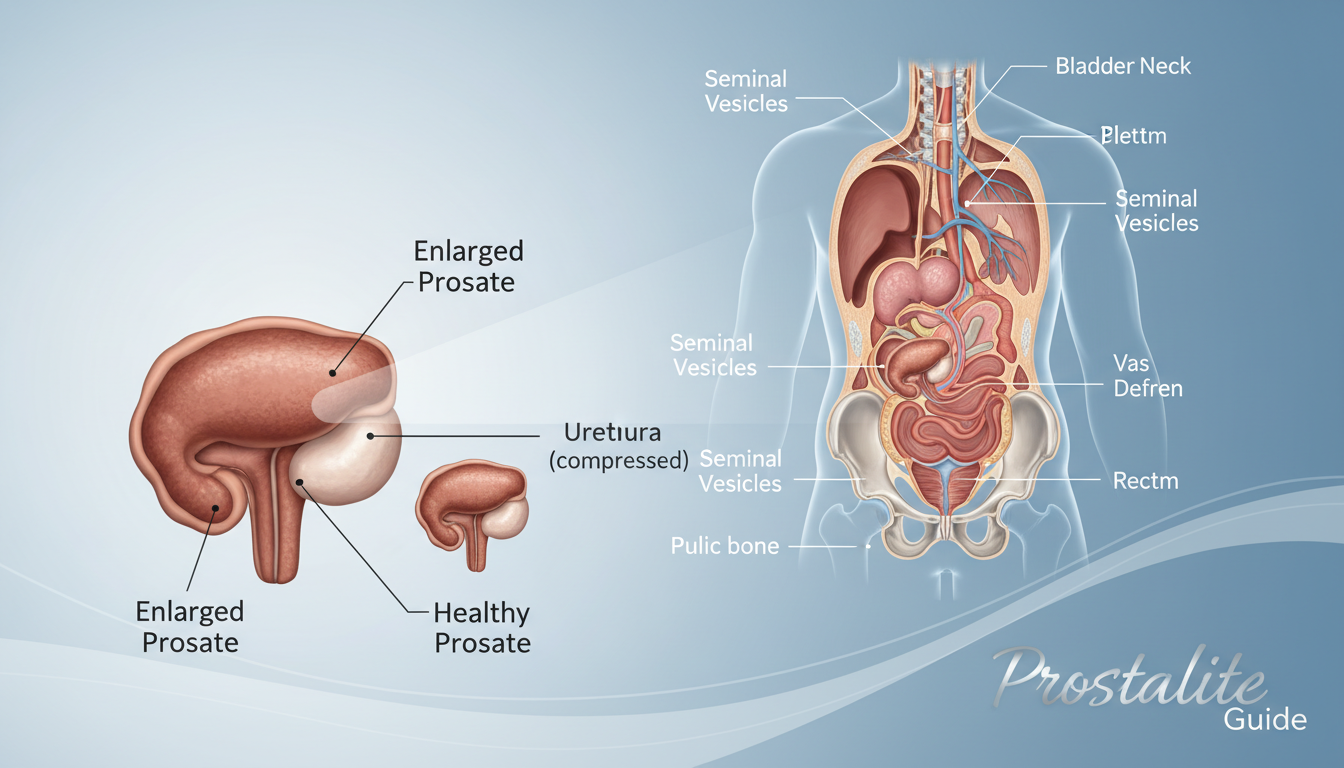
The prostate gland sits just below the bladder and links to the urinary tract. It adds fluid to semen and surrounds the tube that carries urine out of the body.
What the gland does and where it sits
The urethra is the tube that runs from the bladder through the gland to the outside. When the gland grows, it can press on that tube and make urine flow slower or less steady.
What benign prostatic hyperplasia means — and what it does not
Benign prostatic hyperplasia is a noncancerous increase in cell number that makes the gland larger than usual. Benign means it is not cancer, and BPH does not automatically mean someone has cancer or will get it.
How growth can affect the bladder and urine flow over time
As the urethra narrows, the bladder must work harder to push urine out. Over time the bladder muscle can become strained, less effective, and may not empty completely.
“Anatomy and individual response vary, so symptoms differ even with similar gland size.”
How prostate growth can interfere with urine flow
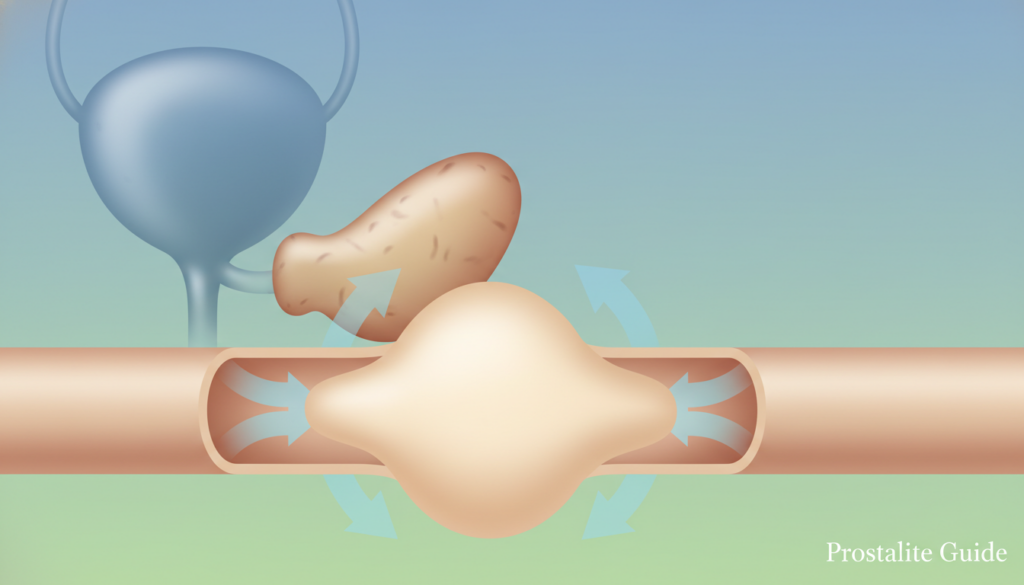
Think of the area like simple plumbing. When tissue around the urinary tube expands, it can narrow the channel that carries urine from the bladder. That narrowing raises pressure at the exit and makes it harder for urine to move freely.
Why pressure on the urethra leads to hesitancy and dribbling
Narrowing of the urethra can cause trouble starting a stream, a weak or slow flow, and stopping-and-starting during urination. After finishing, some people notice dribbling because the channel does not allow a clean, full release.
Why incomplete bladder emptying can develop
Over time, the bladder works harder to push urine past the narrowed area. That extra work can tire the muscle and reduce its ability to empty completely.
Incomplete emptying means a person may feel the need to go again soon. It is not something one can confirm at home with certainty; clinicians use history, exam, and tests to check if obstruction or bladder function is involved.
- Common lower urinary symptoms include hesitancy, weak stream, and dribbling.
- Urgency and frequency can come from a more sensitive or strained bladder.
- Other issues—like infections, neurologic problems, or some medicines—can cause similar patterns.
Track when symptoms occur (day vs night), triggers like caffeine, and how much they disrupt life. That record helps clinicians decide if evaluation or treatment is needed.
Prostate enlargement causes
Most people see gradual tissue growth in midlife that becomes more common with advancing age. This growth often progresses slowly and may not cause symptoms at first.
Age-related growth is the most consistent pattern. Estimates suggest roughly half of men have significant nodular or glandular change by about 60, rising toward 80–90% by the mid-80s. These numbers show how frequently size shifts with advancing years.
Hormonal shifts and what evidence suggests
Research points to changing sex-hormone balance as one contributor. As people age, ratios of androgens and estrogens shift. Those changes may influence how gland tissue grows.
That does not mean a single hormone explains every case. Multiple pathways likely interact, and clinical guidance treats hormones as one piece of the puzzle.
The role of DHT
DHT (dihydrotestosterone) is a potent form of testosterone that acts on gland cells. Studies show DHT can stimulate cell growth, and drugs that lower DHT can reduce gland size or slow further growth.
“DHT-focused treatments exist because of its documented role in promoting cell growth in gland tissue.”
What remains uncertain
Scientists do not yet know why some people’s glands enlarge more than others. Genetics, metabolic health, and lifestyle likely modify risk, but they are not the same as the direct biologic drivers of tissue growth.
| Factor | What is known | How it matters |
|---|---|---|
| Age | Prevalence rises with advancing years | Most common predictor of size changes |
| Hormones | Androgen/estrogen balance shifts with age | May influence cell growth pathways |
| DHT | Stimulates gland cell growth; target of some drugs | Modifying DHT can reduce or slow growth |
| Other risks | Family history, metabolic factors, lifestyle | Increase likelihood but don’t fully explain growth |
Symptoms linked to BPH and when to seek urgent care

Many people notice changes in urination that start slowly and may affect sleep or daily plans. Tracking patterns helps a clinician evaluate whether symptoms are benign or need testing.
Common lower urinary tract symptoms to notice
Common symptoms include frequent trips to the bathroom, a sudden urge to go, waking at night to urinate (nocturia), a weak or slow stream, hesitancy when starting, and dribbling after finishing.
Severity varies. For some, symptoms are a mild nuisance. For others, they cause sleep loss and reduce quality of life. Patterns often change slowly over months to years.
Symptoms that may overlap with other health problems
Similar symptoms can come from a urinary tract infection, prostatitis, bladder conditions, certain medicines, or neurologic issues. Self-diagnosis can be misleading.
Signs that suggest infection or inflammation include pain during urination, fever without other cause, unusual urine odor, or odd urine color. These clues help clinicians choose tests.
Red flags that warrant immediate medical evaluation
Seek urgent care for inability to urinate (acute urinary retention), visible blood in urine, or fever and chills with painful, frequent urination. Significant lower abdominal or urinary tract pain also needs prompt attention.
“Acute urinary retention is a medical emergency and requires immediate evaluation.”
If symptoms are persistent or worsen but do not meet urgent criteria, arrange a timely appointment with a clinician to review options and next steps.
| Symptom | What it might mean | When to seek care |
|---|---|---|
| Frequent urination | Often a sign of lower tract irritation or bladder sensitivity | If daily life or sleep is disrupted |
| Weak stream / hesitancy | May reflect partial obstruction or bladder muscle strain | When it worsens or causes incomplete emptying |
| Blood in urine | Can indicate infection, injury, or other issues | Any visible blood requires prompt evaluation |
| Inability to urinate | Acute retention—bladder cannot empty | Go to urgent care or ER immediately |
Risk factors that can increase the likelihood of benign prostatic hyperplasia
Some traits and health conditions are linked to a higher likelihood of gland tissue growth as people age. A risk factor means only that the chance is higher—not that the factor is a direct cause.
Age over forty and increasing prevalence later in life
Age is the clearest predictor. BPH is uncommon under forty and becomes more likely as men grow older. Clinicians often consider age when deciding whether to screen or evaluate urinary symptoms.
Family history of prostate issues
Having a father or brother with known gland problems raises the risk developing similar patterns. Family history is a practical clue but not proof that someone will have the same outcome.
Health conditions and medications that may be associated in studies
Research shows links between diabetes, heart disease, and higher odds of gland-related symptoms. Certain medicines, including beta blockers in some reports, may be tied to urinary patterns.
These findings are associations and do not prove causation.
Lifestyle factors such as obesity and low physical activity
Obesity and low physical activity are associated with greater chance of gland growth and related symptoms. Improving weight and activity is often part of broader health advice.
- Define a risk: linked to higher likelihood, not proof.
- Talk with a clinician about personal risk and options.
- Lifestyle changes and medication review are common, practical steps.
BPH vs prostate cancer and other conditions with similar symptoms
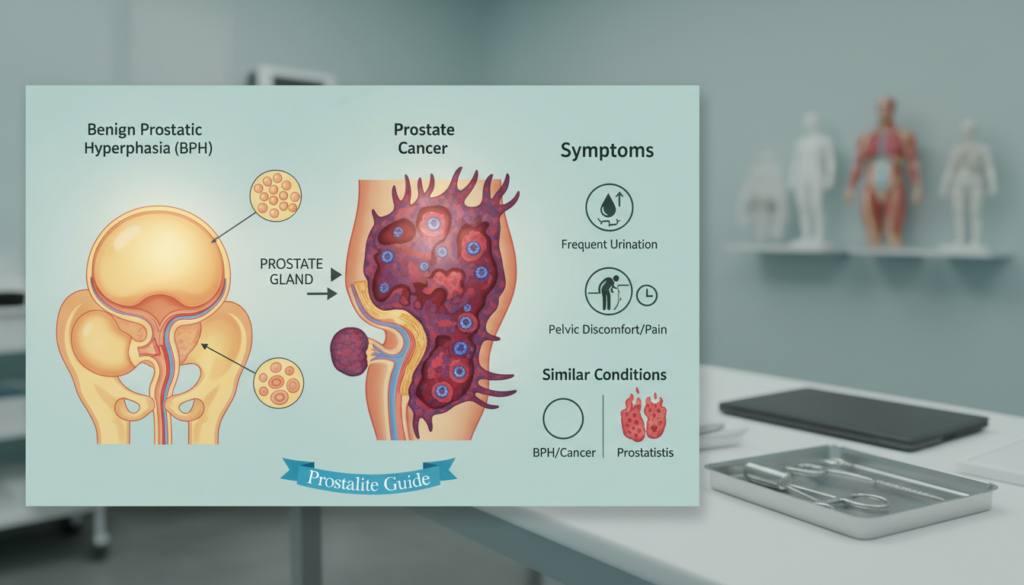
Distinguishing benign prostatic hyperplasia from malignant disease matters because the tests, follow-up, and treatment differ.
Why BPH is benign and doesn’t mean cancer
Benign prostatic hyperplasia is a noncancerous growth of gland tissue. It does not mean a person has prostate cancer and does not automatically raise cancer risk.
Why symptoms still deserve evaluation to rule out other causes
Urinary symptoms overlap across several conditions, including infection, bladder problems, medication effects, and cancer. Similar signs make self-diagnosis unreliable.
- Key distinction: BPH is benign growth; cancer involves malignant cell changes.
- Why confusion happens: both become more common with age and can cause similar symptoms.
- What a doctor will ask: symptom timeline, severity, blood in urine, pain, fever, and medication use.
Practical note: Online information can help someone prepare for a visit, but tests and clinical judgment are needed to separate BPH, infection, bladder problems, or cancer safely.
“Evaluation helps rule out treatable causes and directs appropriate care.”
How clinicians evaluate urinary symptoms and suspected BPH
When urinary changes prompt a visit, clinicians start by mapping a clear timeline of symptoms and daily patterns. A focused history captures day versus night trips, urgency, a weak stream, hesitancy, and any triggers such as caffeine or alcohol.
What the medical history should cover
The clinician asks specific questions about symptom onset, severity, and how sleep or activity is affected. They review all medicines and family history, since drugs can worsen urinary problems or cause retention.
Physical exam basics
A brief exam often includes abdominal and groin checks and a digital rectal exam (DRE). The DRE gives information on size, tenderness, or irregularities but is not a standalone diagnosis.
Common tests used in the U.S.
Typical steps include urinalysis to look for infection or blood and PSA blood testing when appropriate. Imaging (ultrasound), urodynamic studies, and cystoscopy may be used when obstruction or bladder dysfunction is suspected. Biopsy is reserved when cancer must be ruled out.
How results guide care
Test findings help distinguish bladder muscle problems, infection/inflammation, and obstruction at the urethra or bladder neck. Evaluation is individualized; the doctor recommends further testing or treatment based on symptoms, age, and overall health.
“A clear history and targeted testing direct care more than any single exam alone.”
How to talk with a healthcare professional about symptoms
Clear notes on daily patterns give a clinician useful context for urinary concerns. Preparing brief records helps make visits more efficient and ensures important details are not missed.
How to track urinary changes, sleep disruption, and quality-of-life impact
Prepare a 3–7 day bladder diary. Note times you urinate, approximate amounts, fluid intake, and any urgency or leaks. This information paints a clear picture without self-diagnosing.
List all medicines and supplements. Include over-the-counter products and recent changes. Clinicians often adjust plans based on medication details.
- Track sleep: count how many times you wake to urinate and whether sleep is shortened.
- Note impact: record when urgency limits activities or causes accidents.
- Bring a brief timeline: when changes began and whether they are steady or fluctuating.
Useful questions to ask the doctor include: What conditions are being considered? What tests do you recommend? What does watchful waiting involve for mild symptoms?
Share goals and preferences—such as improving sleep or avoiding certain side effects—to support shared decision-making. Report red flags right away: inability to urinate, fever with painful urination, or visible blood in urine.
“Honest, organized information from the patient guides safer, faster decisions.”
Keeping a simple diary and a medication list helps clinicians give focused, practical advice about next steps for overall health.
Evidence-based options that may be recommended if BPH is diagnosed
Clinical guidelines frame options so patients and clinicians can match treatments to goals and health status.
Active monitoring for mild symptoms
Watchful waiting is an active plan for mild symptoms. It involves regular check‑ins, symptom tracking, and tests as needed.
Worsening symptoms or complications such as acute urinary retention may prompt a shift to medical or procedural care.
Lifestyle steps that may help
Simple lifestyle changes can reduce nighttime trips and urgency for some people.
- Limit fluids before bed and reduce caffeine or alcohol in the evening.
- Bladder training and timed voiding to increase control.
- Prevent constipation and maintain regular activity and weight.
Medications: what they do and common side effects
Two main medication classes are used. Alpha blockers relax smooth muscle to ease flow; side effects can include dizziness or low blood pressure. 5‑alpha reductase inhibitors lower DHT and may slow growth over months; hormonal side effects and sexual changes can occur.
Combination therapy is an option for some people but requires discussion about benefits and risks.
Minimally invasive outpatient options and surgery
Outpatient procedures such as the prostatic urethral lift (UroLift) and Rezūm are often same‑day treatments with shorter recovery than major surgery. Long‑term outcomes vary by technique.
Surgery is usually reserved for more severe symptoms or recurrent retention. Common approaches include TURP, TUIP, GreenLight/PVP, electrovaporization, and Aquablation.
“Shared decision‑making balances symptom relief, side effects, and recovery time with the person’s overall health.”
💡 Natural Support Option: Targeting DHT
While medications are common, many men prefer starting with natural support to maintain healthy prostate size. Addressing the root cause—often widely considered to be DHT buildup—is crucial.
We recommend looking for advanced formulas that combine specific herbs known to inhibit DHT. Currently, our top-rated natural option for holistic prostate support is ProstaLite. It uses a high-purity extract designed for maximum absorption and prostate health maintenance.
Check ProstaLite Availability & Price ➤
Conclusion
In summary, gland growth with age often leads to changes in urination that deserve clear attention. ,
The most consistent pattern is age‑related tissue increase that commonly presents as bph or benign prostatic hyperplasia. Pressure on the urethra can reduce flow and, over time, strain the bladder. These changes explain many typical symptoms, including nighttime trips and a weak stream.
Importantly, BPH is benign and not the same as prostate cancer, though similar signs still need evaluation to rule out other problems. Key risk factors include age over 40, family history, obesity, low activity, and some health conditions or medicines.
If symptoms persist, worsen, or disrupt sleep or daily life, consult a clinician. Seek urgent care for inability to urinate, visible blood in urine, fever with painful urination, or severe pain. Tracking symptoms and preparing questions helps a healthcare professional tailor testing and evidence‑based options to fit personal health goals.
Medical Sources and References
This article is based on information from established medical and public health organizations, clinical guidelines, and peer-reviewed research. Key references include publications and patient education resources from:
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) –
- American Urological Association (AUA) –
- National Institutes of Health (NIH) –
- U.S. National Library of Medicine / MedlinePlus –
- National Health Service (NHS, UK) –
- European Association of Urology (EAU) –
The information provided is for educational purposes only and reflects general clinical knowledge at the time of writing. It should not be used as a substitute for professional medical diagnosis, treatment, or individualized care.
FAQ
Why does the prostate gland grow as men age?
What does “benign prostatic hyperplasia” mean and how is it different from cancer?
Where is the gland located and how can growth affect the urinary tract?
How does pressure on the urethra cause weak stream or hesitancy?
Why might incomplete bladder emptying develop with gland growth?
What symptoms commonly signal BPH?
Which symptoms are red flags that require immediate medical attention?
What risk factors increase the chance of developing BPH?
Can lifestyle changes help reduce symptoms?
How do clinicians evaluate urinary symptoms and suspected BPH in the U.S.?
What does watchful waiting involve and when is it appropriate?
What medication options are available and how do they work?
What minimally invasive and surgical treatments exist for significant obstruction?
How can someone prepare to discuss urinary symptoms with a healthcare professional?
Can an infection or other condition cause similar symptoms?
Is blood in the urine always a sign of cancer?

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”