It is a topic most men avoid discussing, even with their doctors. You are already dealing with the frustration of an enlarged prostate (BPH)—the weak stream, the nightly wakings, the urgency. But lately, you have noticed something else.
Your bowel movements have changed. You feel bloated. You are straining on the toilet. You are experiencing gas, discomfort, and chronic constipation.
You start to wonder: “Is this connected? Can an enlarged prostate cause constipation?”
The short answer is YES, but not in the way you might think. It is not just a simple case of “blockage.” It is a complex, interconnected web of anatomy, nerves, medications, and muscle function. In fact, many urologists call this the “Pelvic Vicious Cycle.”
In this comprehensive, medically-grounded guide, we are going to expose the hidden link between your gut and your gland. We will analyze why BPH leads to bowel issues (and vice versa), explore the role of your medication, and provide a complete protocol to fix both problems simultaneously.
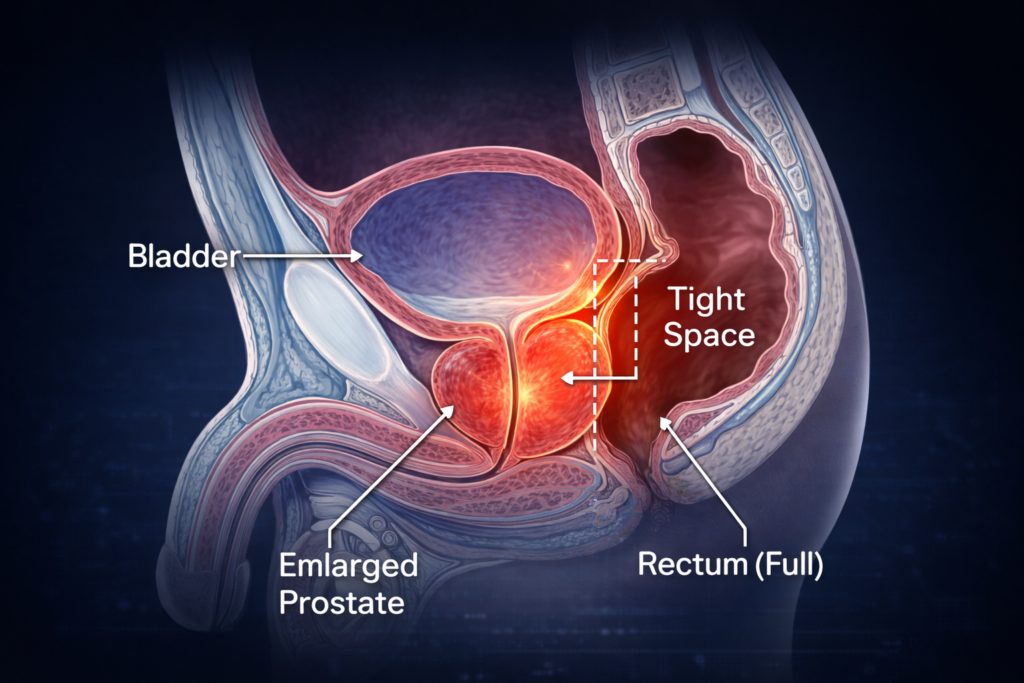
The “Bad Neighbors”: Understanding Your Anatomy
To understand why you can’t poop when you can’t pee, you have to look at the geography of your pelvis. It is a very crowded neighborhood.
The “Thin Wall” Theory
Your prostate gland and your rectum (the lower part of the large intestine) are immediate neighbors. They are separated only by a very thin membrane called the rectovesical septum.
Because they are packed so tightly into the pelvic cavity, a problem with one inevitably affects the other. There is limited real estate down there. If the prostate swells significantly (as it does in BPH), it can physically press backward against the rectum.
While it is rare for a prostate to be so large that it completely blocks the bowel (this usually only happens in advanced prostate cancer), a large benign prostate can create a sensation of “fullness” or “obstruction” that disrupts natural bowel movements.
The Vicious Cycle: How Straining Destroys Your Flow
This is the most critical concept to understand. The relationship between BPH and constipation is a two-way street.
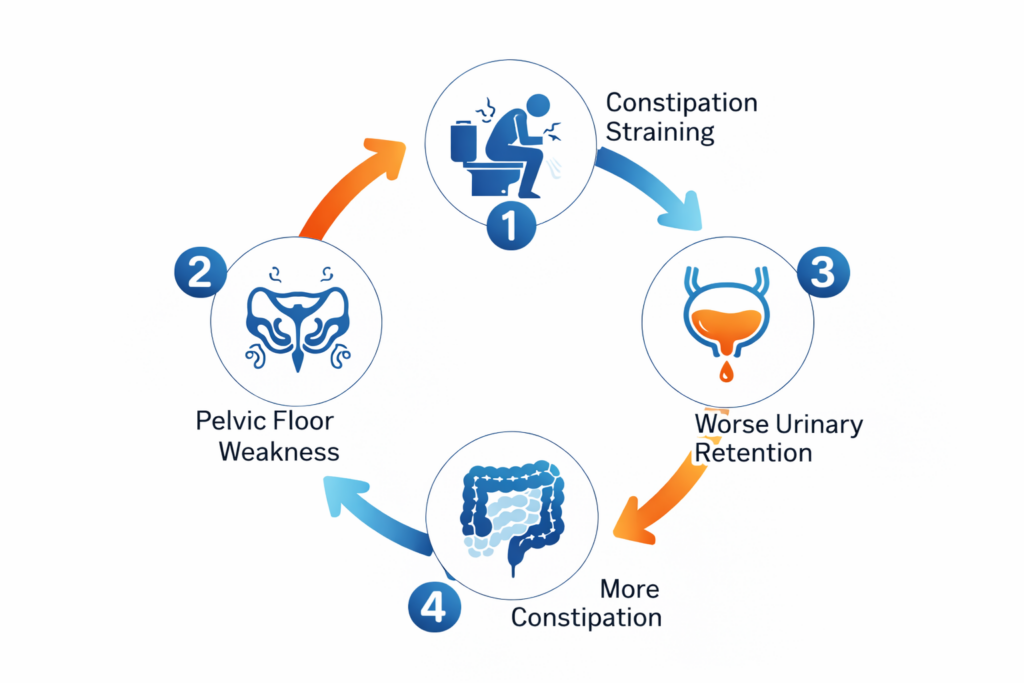
1. The Prostate Affects the Bowel
When you have BPH, you often retain urine. A bladder full of urine pushes against the rectum, making it harder for stool to pass. This leads to constipation.
2. The Bowel Affects the Prostate
This is even more common. When you are constipated, the rectum fills with hard stool. This distended rectum pushes forward directly onto the prostate and the bladder outlet. This extra pressure increases urinary urgency and makes it even harder to urinate.
3. The “Straining” Trap
When you are constipated, you strain. You push hard. This chronic straining weakens the Pelvic Floor Muscles (the same muscles responsible for bladder control). Over time, this leads to Pelvic Floor Dysfunction, where the muscles become too tight or too weak to relax effectively for either urination or defecation.
Can Enlarged Prostate Cause Gas and Bloating?
We often get asked: “Why do I feel so bloated?”
The answer lies in Incomplete Emptying. Whether it is your bladder or your bowels, retaining waste products in the body leads to fermentation and gas production.
- Urinary Retention: Can cause lower abdominal distension that feels like bloating.
- Fecal Retention: Causes bacteria in the gut to over-ferment stool, leading to excessive gas and painful cramping.
If you are experiencing sharp gas pains alongside your urinary symptoms, it is a clear sign that your pelvic floor is in a state of chronic tension.
The Hidden Culprit: Is Your Medication Blocking Your Gut?
Before you blame your diet, check your medicine cabinet. Constipation is a massive, under-reported side effect of standard BPH treatments.

Anticholinergics
Doctors often prescribe these (like Oxybutynin) for “Overactive Bladder.” These drugs work by paralyzing the bladder muscle to stop spasms. Unfortunately, they also “paralyze” the bowel muscles (peristalsis), leading to severe constipation.
Diuretics (Water Pills)
If you take diuretics for high blood pressure, they pull water out of your body. This dehydration turns stool hard and rock-like, making it painful to pass, which in turn aggravates the prostate.
Alpha-Blockers
While generally safer for the gut, some Alpha-blockers used to relax the prostate can cause general fatigue and muscle relaxation that slows down digestion.
When to Worry: Bowel Obstruction vs. BPH
It is crucial to distinguish between simple constipation and a medical emergency. If you experience the following, seek medical help immediately:
- Complete inability to pass gas or stool for 24+ hours.
- Severe, sharp abdominal pain that comes in waves.
- Vomiting along with constipation.
This could indicate a Bowel Obstruction. While BPH alone rarely causes a full obstruction, severe constipation caused by BPH behaviors can lead to fecal impaction.
The Dual-Action Diet: Foods That Fix Both
The good news? The same foods that help shrink the prostate are often the same foods that cure constipation. You need to focus on Fiber and Anti-inflammatory compounds.

1. Flaxseeds (The Golden Bullet)
Flaxseeds are rich in Lignans (which lower DHT levels to help the prostate) and soluble fiber (which softens stool). Adding 2 tablespoons to your morning oatmeal is a game-changer.
2. Prunes and Pears
Grandma was right. Prunes contain sorbitol, a natural laxative. Pears are also excellent. They draw water into the bowel without irritating the bladder.
3. Hydration (The Right Way)
Men with BPH often stop drinking water because they fear the bathroom. This is a mistake. Dehydration makes constipation worse, which makes BPH worse. The trick is to drink water consistently throughout the day but stop 2 hours before bed.
Check out our guide on Prostate-Friendly Drinks for more ideas.
3 Lifestyle Hacks to Break the Cycle
1. The “Squatty Potty” Method
Modern toilets are designed poorly for human anatomy. Sitting at a 90-degree angle kinks the rectum. Using a small footstool to elevate your knees creates a 35-degree angle (squatting), which opens the rectum fully. This reduces the need to strain, protecting your pelvic floor and prostate.
2. Timed Voiding
Don’t wait until your bladder is bursting (which presses on the bowel), and don’t hold in a bowel movement (which presses on the bladder). Go when you feel the urge. “Holding it” is the enemy.
3. Deep Belly Breathing
Stress causes your pelvic muscles to tighten. Practicing deep diaphragmatic breathing helps relax the pelvic floor, making it easier to go #2 without straining.
🔥 Break the Cycle at the Source
You can eat all the fiber in the world, and you can buy the best footstool. But if your prostate remains enlarged, the pressure in your pelvis will never truly go away.
The “blockage” is the root cause.
Imagine trying to drive a car with the handbrake on. That is what your bowel and bladder are doing right now—fighting against the pressure of an enlarged gland.
This is where ProstaLite changes the game. Unlike laxatives that just treat the symptom, ProstaLite is designed to support a healthy prostate size using clinical-grade ingredients like Beta-Sitosterol.
When the prostate shrinks, the pressure releases.
- ✅ No more pressure on the rectum.
- ✅ No more straining to urinate.
- ✅ A relaxed pelvic floor means regular, pain-free movements.
👉 End the “Vicious Cycle” Now – Try ProstaLite
(Exclusive Online Offer – Check Availability)
Frequently Asked Questions
Can an enlarged prostate cause thin stools?
Yes. While less common than constipation, significant prostate enlargement can apply pressure to the rectum, potentially flattening or thinning the stool as it passes through the anal canal. However, thin stools can also indicate other issues, so always consult a doctor.
Does constipation make PSA levels higher?
Indirectly, yes. Constipation can irritate the prostate gland due to proximity. Additionally, a Digital Rectal Exam (DRE) performed when the rectum is full can sometimes yield artificially elevated PSA results due to physical irritation of the gland.
What is the best laxative for someone with an enlarged prostate?
Osmotic laxatives (like Polyethylene Glycol) are generally preferred because they draw water into the bowel to soften stool without causing the aggressive muscle contractions that stimulant laxatives cause, which can irritate the pelvic floor.
Medical References & Sources
- “Lower Urinary Tract Symptoms and Constipation: Is there a link?” – International Journal of Urology.
- “The impact of constipation on BPH symptoms” – American Urological Association (AUA).
- “Side effects of Anticholinergics in elderly men” – Journal of Geriatric Medicine.
- “Dietary fiber and prostate health outcomes” – Clinical Nutrition Journal.

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”