⚡ The Core Difference in 30 Seconds
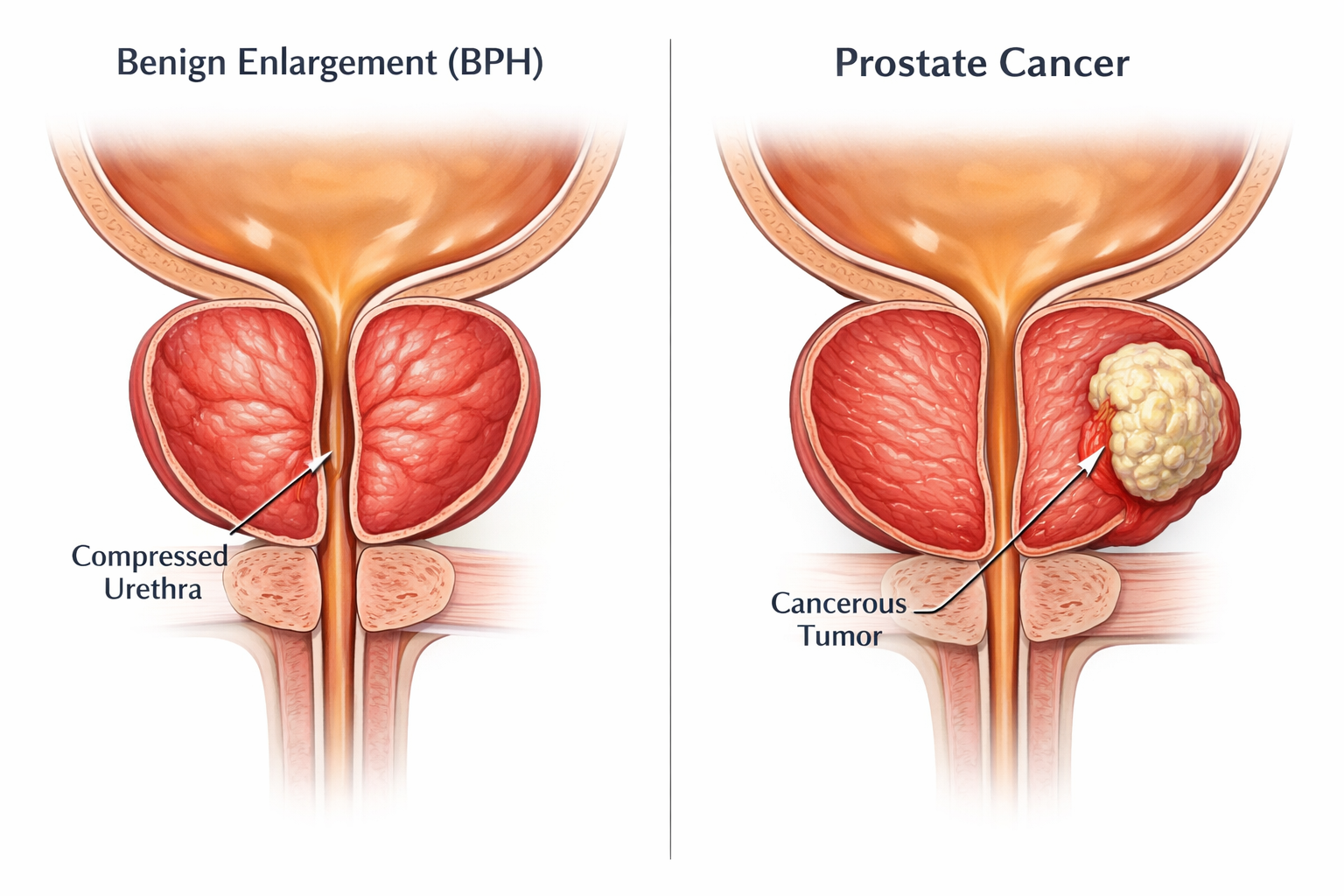
While they share similar symptoms, Enlarged Prostate (BPH) and Prostate Cancer are biologically distinct:
- BPH (Benign): Is an overgrowth of normal cells in the center of the gland. It squeezes the urethra, causing urinary issues. It is NOT cancer and does not spread.
- Prostate Cancer (Malignant): Starts as abnormal cells, usually in the outer part of the gland. It can spread to bones and lymph nodes.
Most men with urinary symptoms have BPH, not cancer. Read on to learn how to tell them apart.
There is perhaps no moment more terrifying for a man than standing in the bathroom at 3 AM, struggling to urinate, and having the thought flash through his mind: “Is this cancer?”
It is a valid fear. Prostate cancer is the second most common cancer in men worldwide. However, there is another condition—far more common and less dangerous—that mimics cancer’s symptoms almost perfectly: Benign Prostatic Hyperplasia (BPH), commonly known as an enlarged prostate.
The confusion between these two conditions causes unnecessary panic for millions of men every year. You might see a high PSA score or feel a “heaviness” in your pelvis and assume the worst. But the reality is often much less frightening.
In this comprehensive guide, we will dissect the difference between enlarged prostate and prostate cancer. We will look at the anatomy, the subtle symptom differences, the diagnostic tests (like the 4K score), and how to manage your health if your diagnosis turns out to be benign.
1. Anatomy 101: Location is Everything
To understand the difference, you have to look inside the gland. The prostate is not just one solid ball; it has zones. Where the growth starts tells doctors a lot about what it is.
The Transition Zone (Home of BPH)
BPH typically occurs in the Transition Zone. This is the inner part of the prostate that surrounds the urethra (the urine tube). Because it is right next to the tube, even a small amount of benign growth here can squeeze the urethra and cause immediate urinary symptoms. This is why BPH is so annoying—it “shuts off the tap.”
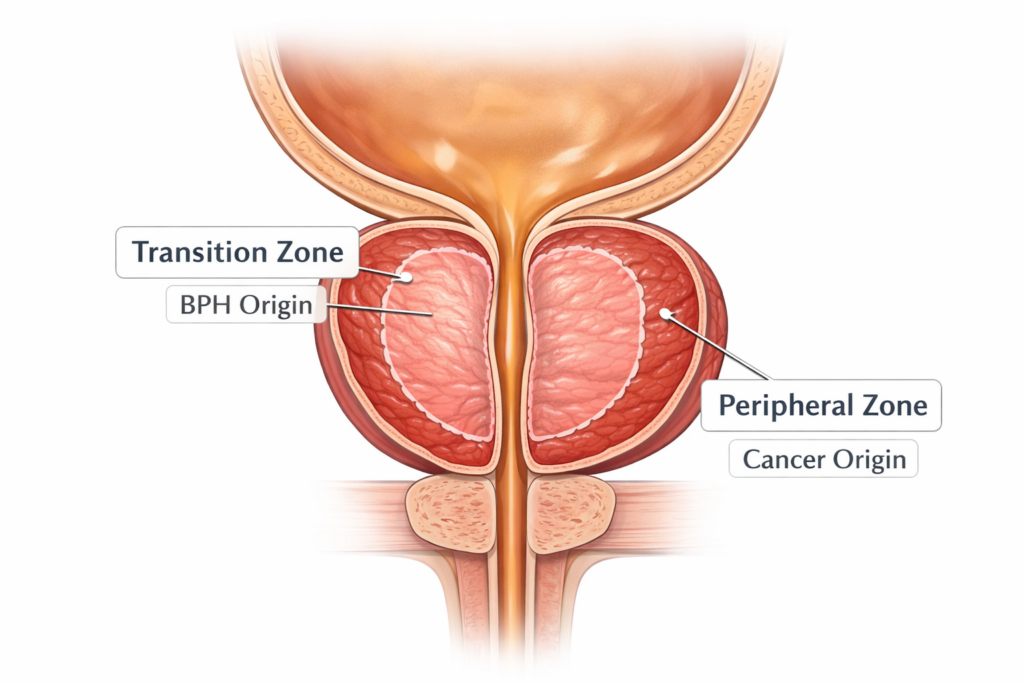
The Peripheral Zone (Home of Cancer)
Prostate cancer usually begins in the Peripheral Zone, which is the outer shell of the gland. Because this area is far away from the urethra, a tumor can grow quite large before it pushes on the tube. This is why early-stage prostate cancer is often silent and has no symptoms at all, whereas BPH is loud and symptomatic early on.
💡 Key Takeaway: Serious urinary symptoms usually point to BPH because of where it grows. Cancer is often quieter in the early stages.
2. The Symptom Trap: Why It’s So Confusing
If cancer grows on the outside, why do people confuse it with BPH? Because eventually, both conditions can affect urination. However, there are subtle differences (“Red Flags”) that you need to watch for.
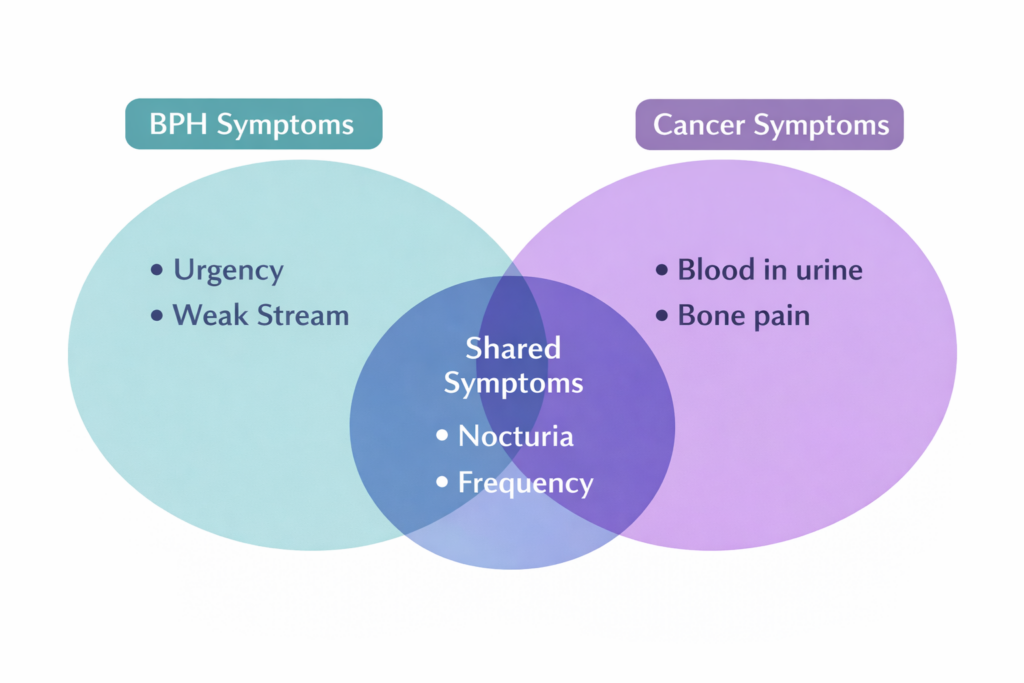
Common Symptoms (Usually BPH, Sometimes Cancer)
- Frequency: Needing to go every 2 hours.
- Nocturia: Waking up multiple times at night.
- Hesitancy: Waiting for the stream to start.
- Dribbling: Leaking after you think you are finished.
The “Red Flags” (More Likely Cancer)
If you experience these, see a doctor immediately, as they are less common in simple BPH:
- Blood in the urine (Hematuria): Never ignore this.
- Blood in semen: A sign of deeper glandular issues.
- Bone pain: Specifically in the hips, back, or ribs (could suggest metastasis).
- Sudden Erectile Dysfunction: While BPH affects sex life, sudden total loss of function can be a nerve signal.
- Unexplained weight loss.
3. The Diagnostic Toolkit: How Doctors Know for Sure
You cannot diagnose yourself based on symptoms alone. Urologists use a specific toolkit to differentiate the two.

The PSA Test (Prostate-Specific Antigen)
This blood test measures a protein produced by the prostate.
The Myth: “High PSA always means cancer.”
The Truth: BPH, infection (Prostatitis), and even riding a bicycle can raise PSA levels. However, extremely high levels or levels that double quickly (PSA Velocity) are concerning.
The 4K Score & Free PSA
Modern medicine has moved beyond just “Total PSA.” Doctors now look at the 4K Score or “Free PSA percentage.”
- High Free PSA (>25%): Usually suggests BPH (Benign).
- Low Free PSA (<10%): Higher risk of Cancer.
The DRE (Digital Rectal Exam)
Since cancer grows on the outside (Peripheral Zone), a doctor can feel it with a finger exam.
- Feels smooth, rubbery, and large? Likely BPH (Adenoma).
- Feels hard, rocky, or asymmetrical? Suspicious for Cancer.
4. What is a “Prostate Adenoma”?
You may see the term “Adenoma” on your MRI report. Do not let this scare you. An Adenoma is simply the medical term for the benign nodules that cause BPH. It is a “tumor” in the technical sense (a swelling), but it is not malignant.
Adenomas are the result of aging and hormonal changes (specifically DHT). They are the physical blockage that stops you from peeing, but they do not spread to other organs.
5. Comparison of Treatment Paths
The biggest difference lies in how we treat them.
| Feature | Enlarged Prostate (BPH) Treatment | Prostate Cancer Treatment |
|---|---|---|
| Goal | Improve quality of life & urine flow. | Remove cancer & extend life. |
| Medication | Alpha-blockers (relax muscles), 5-ARIs (shrink size). | Hormone therapy (ADT) to stop testosterone. |
| Surgery | TURP, Laser, UroLift (minimal invasion). | Radical Prostatectomy (complete removal). |
| Lifestyle | Diet changes & Supplements are highly effective. | Supportive care, but medical intervention is usually required. |
6. Managing Benign Enlargement Naturally
If your doctor confirms that you fall into the “Benign” category (which is the case for the vast majority of men), you might be told to just “Watch and Wait.”
But living with BPH is hard. The constant bathroom trips, the sleep deprivation, and the anxiety can ruin your quality of life. Just because it isn’t cancer doesn’t mean you should suffer.
You can take proactive steps to manage an enlarged adenoma naturally.

🌱 The “Peace of Mind” Protocol
So, the tests came back benign. That’s great news! Now, let’s tackle the symptoms that are still bothering you.
You don’t always need prescription drugs with harsh side effects to manage a benign enlargement. Nature provides powerful tools to support healthy prostate volume.
Enter ProstaLite.
ProstaLite is formulated for men who have ruled out the scary stuff and just want their life back. It uses a scientifically backed blend of:
- ✅ Saw Palmetto: To support hormonal balance.
- ✅ Pygeum Africanum: To help reduce inflammation associated with BPH.
- ✅ Beta-Sitosterol: To improve urine flow and emptying.
Don’t just “watch and wait” while your symptoms get worse. Support your prostate health today.
👉 See How ProstaLite Helps BPH Symptoms
Frequently Asked Questions
Can an enlarged prostate turn into prostate cancer?
No. BPH and Prostate Cancer are two separate conditions. Having BPH does not increase your risk of developing cancer. However, it is possible for a man to have both conditions at the same time.
What is a normal PSA level for a man over 60?
PSA levels rise naturally with age. For men aged 60-69, a PSA range of 0.0 to 4.0 ng/mL is generally considered normal. However, doctors look more at the rate of rise (PSA velocity) than just the single number.
Does bicycling cause high PSA?
Yes. Intense cycling puts pressure on the prostate, which can temporarily spike PSA levels. It is recommended to avoid cycling for 48 hours before a PSA blood test to ensure accuracy.
Is 4k score better than PSA?
The 4K score is considered more accurate than a standard PSA test for predicting aggressive cancer. It combines four specific prostate proteins with clinical data to give a percentage risk score, helping to avoid unnecessary biopsies.
Scientific References
- “Benign Prostatic Hyperplasia vs. Prostate Cancer: Statistics” – American Cancer Society.
- “Prostate Zones and Carcinoma Origin” – Journal of Urology.
- “PSA Testing and BPH Correlation” – National Institute of Diabetes and Digestive and Kidney Diseases.

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”