⚠️ Medical Disclaimer: This article is for educational purposes only. If you experience blood in urine, fever, or severe pain, seek immediate medical attention.
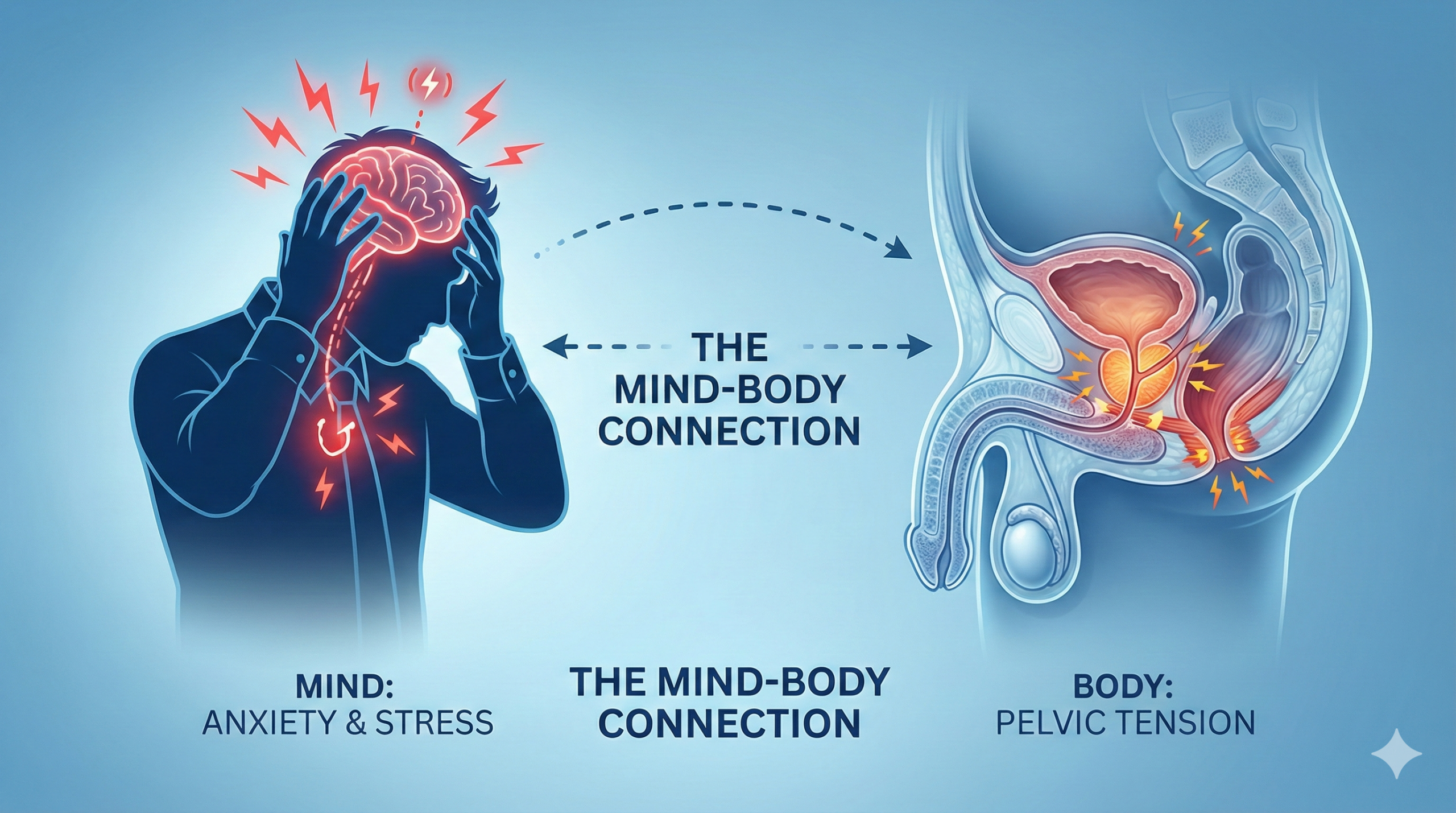
One observational study found that up to 40% of men with pelvic discomfort report heightened symptoms during periods of high emotional strain. This surprising figure shows the scale at which feeling anxious can affect daily life.
Stress, anxiety, and prostate health are defined here for clarity. Stress refers to the body’s response to perceived threats. Anxiety is persistent worry that may change attention to bodily sensations. Prostate health means symptoms linked to the gland but not a diagnosis.
The goal of this article is education, not medical diagnosis. It explains how hormones like cortisol, pelvic floor tension, sleep disruption, and attention to sensations can alter how urinary or pelvic discomfort feels. Individual variation is common; similar sensations can come from many conditions.
If symptoms persist or worsen, readers are urged to consult a healthcare professional for evaluation rather than self-labeling.
Key Takeaways
- Emotional responses can change how pelvic or urinary sensations are perceived.
- Biological pathways include cortisol, adrenaline, and muscle tension.
- Symptoms do not equal diagnosis; many causes may overlap.
- Individual differences mean experiences vary widely among men.
- Seek medical evaluation for persistent or worsening pain.
Understanding prostate discomfort and why “pain” can feel hard to pinpoint
Locating where pelvic pain starts is rarely straightforward, since nearby organs and nerves often blur the origin of sensations.
How discomfort may present: People commonly report pressure, aching, burning, or vague pelvic heaviness rather than a single sharp pain. This makes it hard to identify the exact source.
Where it may be felt: Lower abdomen, pelvic region, perineum, groin, lower back, or during/after urination or ejaculation. Nerves and nearby organs can refer sensations to a different side or area.
Symptoms, risk factors, and underlying causes
Symptoms are what a person feels — urgency, frequency, weak stream, burning, or incomplete emptying.
Risk factors are things that raise the chance of issues, such as age for gland enlargement or past infections.
Underlying causes include inflammation, infection, tissue growth, or pelvic muscle spasm; multiple sources can occur together.
How urinary issues and worry can reinforce each other
LUTS fall into storage (frequency, urgency, nighttime urination) and emptying (weak stream, hesitancy, dribbling). Both can disrupt sleep and daily routine.
Worry and hypervigilance can increase muscle tension and sleep loss, which may make urinary discomfort feel worse over time. Because two men can have similar symptoms with different causes, persistent problems deserve clinician-guided assessment.
Stress and prostate health: what research and clinical guidance suggest about the relationship
Clinical guidance and research point to several biological routes that may explain why emotional arousal can alter lower urinary symptoms. These pathways do not prove direct causation but offer plausible mechanisms clinicians consider when evaluating men with pelvic complaints.
Cortisol, inflammatory pathways, and systemic effects
Cortisol rises when the body senses threat. Clinical sources suggest prolonged high cortisol may be associated with increased inflammatory signaling. This type of inflammation is broad and does not automatically mean infection.
Adrenaline and smooth muscle tone
Acute catecholamine release can tighten smooth muscle. That may change bladder neck and prostate gland tone and make starting or emptying urine feel harder for some men.
Pelvic floor tension and symptom amplification
Anxiety can cause unconscious pelvic floor tightening. Chronic tension may narrow the urethra and contribute to urgency or a sense of incomplete emptying even when no dangerous condition exists.
Hormone shifts and nutrient context
Some sources note that long-term arousal may alter sex hormone balance and DHT conversion, which could influence BPH symptom severity in some individuals. Zinc is concentrated in prostate tissue and is discussed in clinical commentary, but nutrient status is only one factor; diet or supplements should follow professional advice.
“These pathways are associations and suggest possible mechanisms rather than proof of direct cause.”
How stress may affect common prostate-related conditions without being the direct cause

Perception of pelvic discomfort often changes with mood, sleep loss, or bodily tension, which can raise symptom burden.
Benign prostatic hyperplasia and lower urinary tract symptoms
Benign prostatic enlargement is a noncancerous growth that can squeeze the urethra and cause LUTS such as frequency, weak stream, and nocturia.
Age-related prevalence rises sharply: about 50% of men aged 50–60, 70% of those 61–69, and roughly 80% of men 70+ show enlargement in population studies. Emotional factors tend to amplify how bothersome these symptoms feel rather than cause the growth itself.
Prostatitis and why psychological factors may amplify pain and urinary discomfort for some people
Prostatitis covers inflammatory or infection-related syndromes that often cause pelvic pain and urinary change.
Educational resources note that psychological factors can worsen pain intensity and urgency for some patients, though mechanisms remain unclear. Persistent pelvic pain or urinary change should be evaluated, not simply attributed to mood.
Prostate cancer concerns, distress, and the role of screening conversations
Fear of cancer or uncertain symptoms commonly raises anxiety after a concerning test or at diagnosis.
Clinicians can guide appropriate screening and follow-up based on age, risk, and presentation. Distress screening and timely mental health support are recommended parts of comprehensive care after a diagnosis.
Recognizing symptom patterns and knowing when to seek medical evaluation

Recognizing patterns in lower urinary complaints helps separate temporary flare-ups from persistent problems. Simple tracking clarifies what to report at a visit and supports shared decision-making about screening or further testing.
Lower urinary tract symptoms to track
Note which symptoms occur, how often, and what triggers them (caffeine, alcohol, sleep loss, sudden worry). Track disruption to sleep or daily tasks over time.
- Frequency, urgency, nighttime urination (nocturia)
- Weak stream, hesitancy, terminal dribbling
- Sensation of incomplete emptying
Red flags that warrant prompt attention
Seek immediate care for inability to urinate, fever with pelvic pain, visible blood in urine, severe escalating pain, or major unintentional weight loss. Urgent signs should not be dismissed as temporary.
What a clinician may consider
A clinician will review medical history, medications (possible side effects), mental health context, and perform a focused exam. Tests may include urinalysis, a discussion about PSA and screening, or imaging and referral if needed.
Credible information on a website can help patients prepare questions, but diagnosis and treatment options should be decided with the care team. Seeking emotional support alongside medical evaluation is a useful way to manage changes over time.
Some men choose to explore dietary supplements as part of a broader prostate health routine.
If you are considering this option, you can learn more about ProstaLite here, but it should not replace professional medical advice.
Medical References
The information in this article is based on evidence from peer-reviewed research and guidance provided by trusted medical organizations, including:
- Mayo Clinic – Stress, anxiety, and physical symptoms
- Cleveland Clinic – How stress affects the body and pain perception
- National Institutes of Health (NIH) – Stress, inflammation, and chronic pain pathways
- Urology Care Foundation – Prostate health and urinary symptoms
Conclusion
The central point: feelings and bodily signals often interact, so emotional factors may change how urinary or pelvic sensations are felt without proving a direct structural cause.
Readers should keep the symptom–risk–cause distinction in mind. Track what happens, note triggers, and share findings with a clinician. Men with persistent urinary change, worsening discomfort, or red-flag signs should seek timely medical evaluation.
Managing stress and anxiety through sleep, activity, and relaxation can improve quality of life but is complementary to medical assessment and treatment choices. Discuss mood openly with a provider; mental health support and symptom care can work together. For concerns about prostate cancer, pursue individualized screening and clear follow-up plans.
Action: get reliable information, track symptoms, and consult a qualified clinician if problems persist or worsen.
FAQ
Can anxiety cause pain in the prostate area?
Where is prostate-area pain commonly felt?
How can urinary symptoms and anxiety reinforce one another?
What does research say about cortisol and inflammation in prostate conditions?
Can adrenaline and “fight-or-flight” responses change bladder or pelvic muscle tone?
Why does pelvic floor tension make urinary discomfort worse?
Do hormone shifts during chronic anxiety affect benign prostatic enlargement (BPH)?
Are there nutritional factors linked to prostate tissue and symptom management?
How can mental health interventions help men with urinary or pelvic complaints?
Can anxiety cause prostatitis-like symptoms?
Should men with family history of prostate cancer be more concerned about symptom-related anxiety?
What lower urinary tract symptoms should men monitor?
What red flags warrant urgent medical attention?
What will a clinician consider during evaluation of pelvic or urinary complaints?
What nonmedical self-care strategies can reduce symptom intensity?
How do treatments differ between benign enlargement, prostatitis, and anxiety-driven pelvic pain?

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”