⚠️ Medical Disclaimer: This article is for educational purposes only. If you experience blood in urine, severe pain, or inability to urinate, seek immediate emergency care.
Fact: Death rates for prostate cancer fell by about half from 1993 to 2013 before leveling off, reflecting major gains from early detection and treatment.
This introduction explains what “prostate warning signs” means in practical terms. It refers to changes a person may notice, especially urinary or sexual symptoms, that should prompt a clinical conversation. Many causes are benign, but persistent or worsening issues deserve evaluation.
The guide will show what to watch for, how to describe changes clearly, and when to seek timely care. Clinicians use history, exam, and tests to identify the underlying cause rather than assuming cancer.
Why this matters: prostate cancer is common among men, and early assessment can improve outcomes. Clinicians consider the full picture — severity, duration, age, and personal risk — before advising next steps. If symptoms are severe, such as inability to urinate or heavy bleeding, urgent evaluation is reasonable.
Key Takeaways
- Early evaluation helps find the cause, which can be benign or serious.
- Noticeable urinary or sexual changes often prompt a visit to a doctor.
- Symptoms alone do not equal cancer; testing clarifies the diagnosis.
- Clinicians weigh severity, duration, age, and risk factors when advising care.
- Seek urgent care for severe problems like inability to urinate or heavy bleeding.
Why paying attention to prostate symptoms matters over time
Understanding how changes develop over time helps people decide when to ask a clinician for an evaluation.
What the gland does
The small gland sits below the bladder and helps make fluid that mixes with sperm. Its position around the urethra explains why growth or inflammation can affect urination.
How cancer can start
Cells in the gland can acquire changes that let them grow without the usual limits. This process may take years and varies from person to person.
What research and guidance show
Early diagnosis is often linked with better outcomes. Death rates for prostate cancer fell by about half from 1993 to 2013 and then stabilized, which may reflect more later-stage diagnoses in some groups.
Why growth rates differ
Some prostate cancer types grow slowly and may never need immediate action. Others spread faster and move through stages that change the evaluation and management approach. Treatment decisions depend on age, health, and test results.
| Feature | Slow-growing | Faster-growing |
|---|---|---|
| Typical course | Long, watchful follow-up | Shorter interval to active care |
| Tests used | Monitoring and periodic assessment | Imaging and biopsy for confirmation |
| Clinical focus | Balance risks and quality of life | Timely diagnosis and intervention |
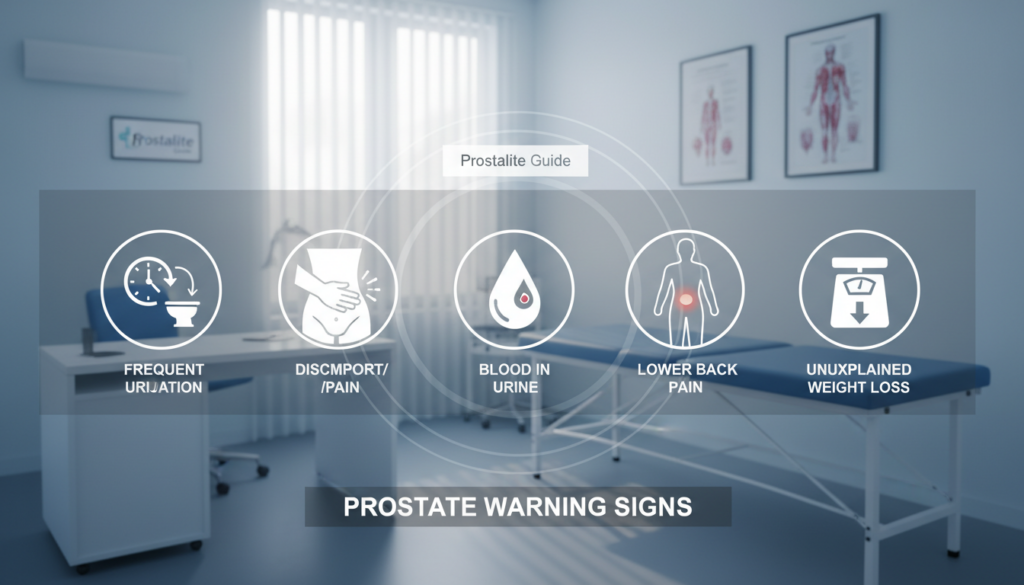
Prostate warning signs that may warrant a medical evaluation

Not every change in bathroom habits means serious illness. However, new or worsening symptoms that disrupt sleep or daily life should prompt a discussion with a clinician.
When to consider evaluation
Frequent urination or nocturia: waking several times at night or a clear increase in daytime trips to the bathroom is worth tracking.
Starting, stopping, or incomplete emptying
Hesitancy (difficulty starting) and intermittency (stopping and starting) may signal obstruction or other conditions. A constant feeling that the bladder is not empty is also important if it lasts.
Weak or interrupted flow
A reduced stream can reflect narrowing near the urethra. Multiple conditions can cause this; persistent change deserves evaluation.
Pain, burning, or blood
Discomfort or burning during urination often points to irritation or infection. Blood in urine or semen should prompt prompt medical review to find the source.
“New, persistent, or worsening urinary problems are reasons to seek care rather than assume the cause.”
Preparing for the visit
- Note timing (day/night), duration, and severity.
- Record related fever, pelvic or back pain, or sexual changes.
- Seek same-day care for inability to urinate, severe pain with fever, or heavy bleeding.
What these signs can be linked to besides cancer
Many different conditions can produce similar urinary or pelvic complaints, so clinicians look beyond symptoms.
Why overlap happens: Growth, inflammation, infection, or unrelated bladder issues can each cause hesitancy, weak flow, or a sense of incomplete emptying. The same complaint does not mean a single disease.
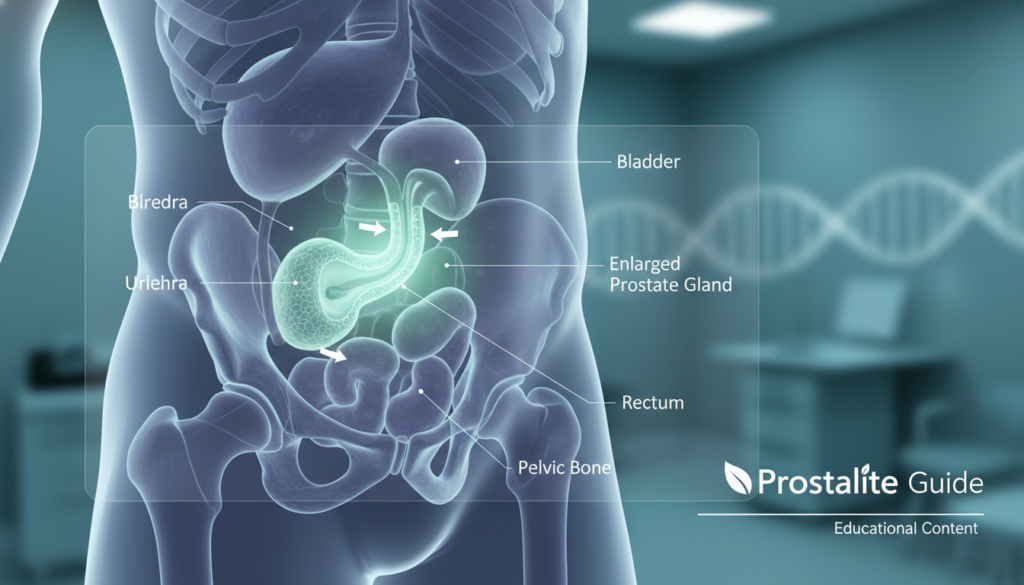
Benign prostatic hyperplasia and flow changes
Benign prostatic hyperplasia (BPH) refers to non-cancer enlargement that can compress the urethra. This hyperplasia may produce gradual changes like reduced stream or incomplete emptying.
Longer-term, slowly worsening issues often point toward enlargement rather than an acute infection.
Prostatitis and inflammation or infection
Prostatitis means inflammation of the gland and can be infectious or non-infectious. It often causes more abrupt discomfort, burning, or pelvic tenderness and sometimes fever.
Sudden onset with fever or marked discomfort more commonly suggests infection or inflammation than slow growth.
“The same symptom can have several causes; evaluation determines which is most likely.”
How clinicians decide: Timing, associated features, age, medications, and other bladder conditions shape the assessment. Tests help distinguish benign prostatic hyperplasia, prostatitis, and other conditions from cancer.
- Sudden fever and marked pain often point to infection.
- Gradual flow changes often suggest enlargement or obstruction.
- Even with benign causes, clinicians may discuss prostate cancer risk and screening when appropriate.
Who may be at higher risk and when screening discussions come up

Certain personal traits raise the chance that a man will develop cancer and prompt an earlier screening conversation.
Risk factors clinicians commonly consider
Risk factors are characteristics—like older age, a close family history (father or brother), or being an African American man in the United States—that may increase risk.
How risk differs from symptoms
Risk is about probability before symptoms appear. Symptoms are changes a person notices later.
A man can have urinary problems from benign causes yet have low cancer risk, or be at higher risk with no symptoms. Both matter when deciding care.
Talking about screening and PSA
PSA (prostate-specific antigen) is a blood test used in screening. PSA levels can rise for many reasons and are not cancer-specific.
Clinicians may also offer a brief digital rectal exam. Decisions about screening use shared decision-making—discussing benefits, harms, and follow-up options.
“Discuss baseline risk, testing choices, how results are interpreted, and likely next steps.”
If testing or symptoms lead to further evaluation, diagnosis and treatment choices vary from active monitoring to more intensive therapy based on health, results, and preferences.
Conclusion
Persistent urinary changes, blood in urine or semen, and ongoing pelvic pain merit timely evaluation. These signs often reflect benign conditions but can also require focused assessment of the prostate.
The goal of a visit is to clarify the cause, not assume cancer. A clinician will discuss possible tests and treatment options based on findings and individual risk.
If problems persist, worsen, or disrupt sleep and daily life, contact a doctor for guidance on evaluation and next steps. People with higher risk by age, family history, or race may raise screening discussions earlier.
For urgent issues such as inability to urinate or heavy bleeding, seek prompt care. Tracking symptoms and sharing clear details helps clinicians support better long-term health.
Medical References
This article is informed by clinical guidance and peer-reviewed research from trusted medical organizations, including:
- Mayo Clinic – Prostate cancer symptoms and diagnosis
- Cleveland Clinic – Benign prostatic hyperplasia and urinary symptoms
- National Cancer Institute (NCI) – Prostate cancer screening and symptoms
- Urology Care Foundation – Prostate health and urinary symptoms
FAQ
When should someone see a doctor about urinary or pelvic changes?
Why does paying attention to these symptoms matter over time?
What does the prostate gland do and how can disease begin there?
What does research say about early detection and outcomes?
Why do some cancers progress slowly while others spread faster?
Which urinary changes should prompt evaluation?
What does weak or interrupted urine flow indicate?
How concerning are pain or burning during urination?
What does blood in urine or semen mean and how urgent is it?
When do symptoms become an emergency?
What other conditions can cause similar symptoms besides cancer?
What is benign prostatic hyperplasia and how does it affect urine flow?
How does prostatitis present and how is it treated?
Who is at higher risk and when should screening be discussed?
How does “risk” differ from “symptoms” and why do both matter?
What role does prostate-specific antigen testing play in screening?
What tests might follow an abnormal exam or PSA result?
Taking Action for Your Prostate Health
Recognizing warning signs is an important first step. When a healthcare professional confirms that symptoms are related to benign prostate changes rather than a serious condition, some men choose to explore supportive lifestyle and wellness options.
As part of a broader prostate health routine, certain dietary supplements are sometimes considered. Ingredients such as Saw Palmetto and Beta-Sitosterol have been studied for their potential role in supporting normal urinary function, although results can vary between individuals.
If you are interested in learning more about this category of supplements, you can review information about ProstaLite here. This product is not intended to diagnose, treat, cure, or prevent any disease and should not replace professional medical advice.

“Abdullah is a dedicated health researcher specialized in urological wellness and prostate health. With years of experience in analyzing clinical studies, he provides evidence-based guidance to help men lead healthier lives.”


